

May 2015
IN THIS ISSUE:
![]()
- Computer-assisted detection of tumors helps identify subtle forms of spinal cancer
- Maryland Senator Ben Cardin and CNN's Sanjay Gupta address NIH staff
- Valerie Jarrett, senior advisor to the President, emphasizes importance of minority health
- Cameras, analysis software offer new ways to view the torso
- Employees keep their wheels spinning on the way to work
- Take the Federal Employee Viewpoint Survey by June 12 to influence change
- Frankie and Me: Yale doctor lectures on personal and professional prospective on autism
- Patricia Reilly joins the Clinical Center as chief of the ethics office
- Dr. Thomas Fleisher recognized for contribution to clinical immunology
- Social work department honors fellow employee with inaugural award
- What does a depressed brain look like? NIMH studies hope to learn more, recruiting volunteers
- Upcoming Events
Print this Issue ![]() (352 KB)
(352 KB)
ABOUT CC NEWS:
![]()
Published monthly by the Office of Communications and Media Relations. News, article ideas, calendar events, letters, and photographs are welcome. Submissions may be edited.
Clinical Center News
National Institutes of Health
Building 10, 10 Center Drive
Room 6-2551,
Bethesda, MD 20892-1504
Tel: 301-594-5789
Fax: 301-402-0244
Molly.hooven@nih.gov
QUICK LINKS:
![]()
Computer-assisted detection of tumors helps identify subtle forms of spinal cancer
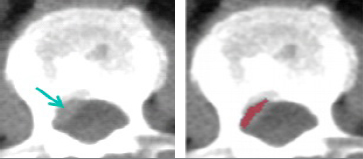 |
These CT images show an epidural mass. The arrow on the left image points to the mass in the spinal canal. The mass is about a quarter of an inch thick. The spherical shading in the right image shows the location and size of the epidural mass with help from the computer-aided detection system. Radiologists can easily miss epidural masses due to their small size and subtle shade. Photo courtesy of Dr. Jiamin Liu. |
The Clinical Center Radiology and Imaging Sciences Department has recently developed a computer system that interprets a computed tomography (CT) scan to better detect tumors in the spinal canal. By utilizing this new computer-assisted detection (CAD) of tumors, doctors at the NIH are able to find and prevent small masses from compressing the spinal cord, which can often lead to paralysis, pain and loss of function in the bladder and bowels.
Studies have shown that treatment of these tumors, including chemotherapy, radiation therapy and sometimes surgery, is well-tolerated even with patients who have been given a limited prognosis. Treatment has resulted in substantially improved quality of life, which supports the need for improved early detection on imaging.
Epidural tumors are so small and subtle on CT images that they are easily missed, even by trained radiologists. In fact, detection of these masses on a CT scan is commonly incidental. The tumors are normally detected by MRI scans when there is preexisting suspicion of their presence. Because half of the studies conducted by the Radiology and Imaging Sciences Department are with patients who already have a known form of cancer, the scientists here decided that identifying these masses before they became symptomatic would be a constructive topic of research.
"Since many of our patients already have cancer, it is important that we can detect masses quickly, including those that affect the spinal cord," said Dr. Ronald Summers, senior investigator in the Imaging Biomarkers and Computer-aided Diagnosis Laboratory within the department. "Our CAD system acts as an automated additional reviewer of CT examinations so that these subtle tumors are less likely to be missed. This project demonstrates how the Clinical Center provides ideal conditions for the development and validation of new technology in the clinical setting."
The computer-assisted detection system scans the spinal canal for epidural tumors through the use of the CT scans. Epidural tumors are on the dura, a thick membrane that surrounds the spinal cord and spinal nerve roots.
Compression of the dura by a tumor can lead to compression of the encompassed spinal cord and nerves. The program is then able to tell physicians where the masses are located. Staff scientist Dr. Jiamin Liu and Imaging Sciences Training Program fellow Dr. Lauren Kim from Summers' Radiology and Imaging Sciences lab are currently working on a study which assesses how well the program works for Clinical Center patients.
Epidural masses are one type of skeletal complication in cancer patients. Others include bone metastases and fractures. Summers' lab is working on automated detection of these abnormalities as well.
Computer-assisted detection is also being used by Summers to identify cancerous tumors in other various regions of the body in addition to the spine, including the colon, ovaries and pancreas.
Maryland Senator Ben Cardin and CNN's Sanjay Gupta address NIH staff
|
|
Valerie Jarrett, senior advisor to the President, emphasizes importance of minority health
On April 14, Valerie Jarrett, senior advisor to President Barack Obama, traveled to the NIH to participate in a commemorative event celebrating 100 years of National Minority Health awareness. Jarrett shared her belief that "diversity is a strength," and voiced her theories on diversifying the field of biomedicine by continuing to create a family friendly workplace for the 21st century worker to thrive, as well as to further address the issue of pay disparities. Additionally, she spoke about precision medicine and the administration's excitement over NIH's efforts. The event was organized by the NIH National Institute on Minority Health and Health Disparities. HHS employees, view the videocast. |
Cameras, analysis software offer new ways to view the torso
Within the NIH Clinical Center's Rehabilitation Medicine Department, Dr. Scott M. Paul, a physical medicine and rehabilitation physician (also known as a physiatrist) is conducting a clinical trial to evaluate stereophotogrammetry as a tool for studying physical deformities.
Stereophotogrammetry generates a three-dimensional image of a patient using four sets of digital camera pods and analysis software.
The existing methods for observing patients with scoliosis and other related chest and back conditions require either the use of x-ray scans, which expose patients to ionizing radiation, or MRI scans, which often require sedation of the patient and provide an altered view of spinal curvature since a patient lies flat in the machine, negating the effects of gravity.
"These are the challenges of studying spine curves: you only get a two-dimensional view via x-ray or an altered three-dimensional flat view with a CT or MRI," Paul said. "Stereophotogrammetry offers the potential to quickly provide 3-D views of spinal curvature of a standing patient without exposing that patient to the radiation of an x-ray."
Within each of the four camera pods used in stereophotogrammetry are two black and white cameras which serve as 'eyes' to build a 3-D image, a color camera to provide surface tone, a strobe light for camera flash and a projector that displays a complex speckled pattern on the surface of the subject. This speckled pattern is a vital component of the project and is what the software program 'reads' to build the image.
"Take our eyes for example. We see slight differences from one eye to the other. This is called parallax and that is how you see in 3-D," Paul explained. "The cameras do the same thing to build the 3-D digital image in 360 degrees."
The second component of the study is MatLab-based analysis software adapted from a program developed by research partners at the University of Alberta in Canada. The software creates 2-D torso slices through the 3-D image (similar to CT or MRI), which are then analyzed using symmetry analysis algorithms. The hope is that these output values will provide meaningful information about the torso and any changes that occur over time.
"Basically, in stereophotogrammetry, we are not looking at the bones themselves. We're looking at the surface. We believe we can extrapolate data from that surface image back to the bones," Paul said.
The goal of the study is to refine the stereophotogrammetry process by collecting images and body data from healthy volunteers and patients with skeletal curvature and other bone conditions in the torso. Subsequently, researchers plan to apply similar algorithms to understand the differences in distribution of fat in individuals who are overweight or obese.
Paul and his team have already completed phase one of the trial and scanned 100 healthy volunteers over the course of two years. In phase one, they found that there was little variability between the results of volunteers who did not have spinal curvatures. This is what would be expected when comparing two healthy people and thus confirmed the stability of the stereophotogrammetry system.
"If there had been too much difference between the scans of healthy volunteers, it wouldn't have been reliable to use the technique to see the difference between a healthy volunteer and patient with scoliosis," said Anne Geller, a post baccalaureate Intramural Research Training Award researcher working on the trial.
The study is now in phase two and Paul is in the process of enrolling patients already diagnosed with scoliosis and other spine and chest conditions.
The team is prepared to enroll up to 150 patients to scan using stereophotogrammetry. The study will see if the system can distinguish a healthy volunteer from a volunteer who has scoliosis and how those results compare to the x-rays. The study will hopefully prove this technique can be used to track and monitor changes in physical deformities over time.
"We are trying to develop a reliable technique that can be used across the spectrum," Paul said.
 |
The camera pods used in stereophotogrammetry contain black and white cameras to help build a 3-D image (image a), a projector that displays a complex speckled pattern on the person's body surface which is read by a software program to create the image (image b) and a color camera to provide surface tone (image c). |
Employees keep their wheels spinning on the way to work
 More than 100 employees from the Clinical Center and nearly 500 from across campus joined in the NIH 8th annual Bike to Work Day May 15. The event promotes and celebrates cycling as a low-cost, healthy, convenient and environment-friendly means to get to work.
More than 100 employees from the Clinical Center and nearly 500 from across campus joined in the NIH 8th annual Bike to Work Day May 15. The event promotes and celebrates cycling as a low-cost, healthy, convenient and environment-friendly means to get to work.
According to Dr. Vernon E. Anderson, a chair of the NIH Bicycle Commuter Club [disclaimer] who works at the National Institute of General Medical Sciences, most NIH cyclists' bike an average of about four miles to work but some travel up to twenty-five miles, coming from Columbia, Md. and several areas throughout Virginia.
"I bike to work for a couple reasons: it's a healthy alternative to the metro as well as a more environmentally friendly one and it's nice to get out and enjoy the weather (rain or shine!)," said David Ichikawa, a technician working in the Clinical Center for the National Institute of Allergy and Infectious Diseases. Ichikawa is featured on the cover of this month's CC News. "Working at the NIH and being surrounded by research aimed at improving health has certainly played a role in pushing me to maintain my health."
Bike racks can be accessed in the Clinical Center underground parking garage and outside the B1 cafeteria. There are showers also available throughout the building.
On Bike to Work Day, A Pit Stop Station was located at Building 1 in the morning for bicyclists to receive refreshments, giveaways, biking information, T-shirts (to pre-registered participants) and to be cheered on by fellow participants and NIH staff. The event was sponsored by the Washington Area Bicycle Association. Learn more: www.biketoworkmetrodc.org [disclaimer].
Take the Federal Employee Viewpoint Survey by June 12 to influence change
Now is the time for federal employees to participate in the Office of Personnel Management (OPM)'s annual 2015 Federal Employee Viewpoint Survey (FEVS). All permanent federal employees who have been onboard as of October 2014 have received an email from OPM to participate in this online, confidential survey through June 12. This is your chance to share concerns and influence change. Take the time to fill out this anonymous survey and let your opinions be heard.
Keep an eye out for more information posted on the Clinical Center intranet website, atrium TV screens, posters and emails from Clinical Center leadership. View past surveys and survey support contact information.
Frankie and Me: Yale doctor lectures on personal and professional prospective on autism
 |
Dr. Kevin Pelphrey and his daughter Frankie as shown in his presentation. |
On April 6, in recognition of National Autism Awareness Month, Dr. Kevin Pelphrey from the Yale School of Medicine presented on how the social brain of a child with an autism spectrum disorder begins to process social information. Pelphrey shared his professional experience and personal experience, as a father of two children with autism.
Pelphrey, who serves as the director of the Yale Center for Translational Developmental Neuroscience, originally focused his studies on basic developmental studies and social cognition but shifted specifically to autism spectrum disorders after his daughter, Frances, was diagnosed with autism around the age of four.
"[Autism is] such a complex problem," he said. "What we don't know enough about is how treatments work – particularly behavior treatments in autism."
He spoke about an imaging study he conducted with children on the autism spectrum and their unaffected siblings – something he's familiar with since his daughter has two brothers, one with autism and one without. "It's a family affair," he said, as he also has nieces and nephews with autism within his extended family. The study allowed him to use imaging techniques to look for regions in the brain that show dysfunction in children with autism compared to both unaffected siblings and typically developing children; look at regions of the brain where unaffected siblings and the child with autism share dysfunction; and examine what areas of the brain help avoid or compensate for that genetic risk of autism.
While relaying the seriousness and importance of continued research, Pelphrey kept a light heartened nature, and even joked that "one of the best ways to avoid autism is to be a girl."
Currently, most of the autism brain imaging studies published are focused on boys. However, Pelphrey and a team of researchers from institutions across the country hope to soon publish results of a study that has a specific focus on girls and the integration of genetics, imaging and behavior.
"It's one of the largest collections of girls with autism and their unaffected siblings," he said.
Pelphrey also touched upon treatment research that could involve experimental therapeutics combined with an administered drug, such as oxytocin – which has shown promising results. Ultimately, he says the question to keep in mind is, "What can I know from science that would allow us to develop better treatments?" Pelphrey and his research team view their findings – linking brain phenotype, genes and social behavior in children with autism – as ways to expand their understanding of autism spectrum disorders and as progressive stages in potential treatment.
The lecture was presented by the National Institute of Mental Health and the Office of Autism Research Coordination. Watch the videocast.
Patricia Reilly joins the Clinical Center as chief of the ethics office
 |
Patricia Reilly, who has served at the NIH for 17 years, joined the Clinical Center in April. |
The Clinical Center recently welcomed Patricia Reilly as the new chief of the Ethics Office, which provides information to employees on issues related to fostering adherence to ethical standards of conduct and the prevention or resolution of conflicts of interest.
"I'm very excited to get to know the people and the program and to build collaborations as a partner with employees at the Clinical Center," said Reilly.
She has served the NIH for about 17 years in a variety of roles including Deputy Director of the Ethics Office within the National Heart, Lung, and Blood Institute and an ethics specialist in the NIH Office of the Director's Office of Ethics.
Dr. Thomas Fleisher recognized for contribution to clinical immunology
 |
Dr. Thomas Fleisher, right, accepts the award April 11 at the annual conference. |
On April 11, Dr. Thomas Fleisher, chief of the Clinical Center Department of Laboratory Medicine, received the 2015 Clinical Immunology Society Presidential Award.
Fleisher was selected by the society for his outstanding dedication and contribution to the field of clinical immunology. Fleisher has been with the NIH for more than three decades and started the immunology laboratory in 1983.
He focuses on disorders of immune function and in particular diseases that are inherited that involve alteration to the way the immune system works.
Social work department honors fellow employee with inaugural award
 |
Schendell Lindsay, Maria Radulovic, Ann Sloane, Nicole Pascua (award winner), Heather Hill and Lynn Hardesty gather at the award ceremony. |
The Social Work Department presented the first Deborah Dozier Hall Award for Professional Development to LT Nicole Pascua. The award honors the memory of social worker Deborah Dozier Hall who served at the NIH for over 20 years and passed away in 2012.
Hall served as Pascua's social work field instructor and mentor. Members of Hall's family attended the award presentation, held during March's Social Work month celebration.
Pascua was recognized for her impact on social work training in the department, on staff members for whom she has served as mentor and teacher and on the social work community through her commitment to educational activities.
What does a depressed brain look like? NIMH studies hope to learn more, recruiting volunteers
- An inpatient research study is assessing the effectiveness of the oral medication diazoxide (an enhancer of glutamate transporter function) versus placebo to rapidly improve hard-to-treat major depressive symptoms. The study enrolls eligible participants ages 18-65, who are diagnosed with major depressive disorder, have previously failed to respond to treatment and are free of other serious medical conditions. This study can last up to 12 weeks and is conducted at the NIH Clinical Center in Bethesda, Md. (Protocol 14-M-0041)
- A brain imaging study will try to see if depressed individuals, ages 18 and older with major depressive disorder, have increased inflammation in their brain. The study involves four outpatient visits or a brief inpatient stay at the NIH Clinical Center in Bethesda, Md. Procedures include blood tests, medical evaluations and two brain scans (PET & MRI Images). Participants do not need to stop their current medications. Those not eligible to participate include pregnant women, current smokers and individuals with serious medical conditions. (Protocol 13-M-0100)
- Studies are enrolling eligible participants ages 18-65 with unipolar or bipolar depression symptoms for a two to three month inpatient stay. The study compares ketamine, an experimental medication, to placebo and evaluates rapid reduction of depressive symptoms (within hours). (Protocol 04-M-0222)
There is no cost to participate in these studies. Eligible participants locally and from around the country may enroll in the studies. Travel arrangements are provided and costs are covered (arrangements vary by distance). After completing a study, participants receive short-term follow-up care at the NIH while transitioning back to a provider. More details: moodresearch@mail.nih.gov, 1-877-MIND-NIH (1-877-646-3644) or TTY 1-866-411-1010, http://www.nimh.nih.gov/labs-at-nimh/join-a-study/adults/adults-depression.shtml.
Upcoming Events
Most lectures will be streamed live and archived
8th Annual NIH Take a Hike Day
June 4, 2015, 11:30 a.m. - 1:30 p.m.
NIH Campus
All NIH employees and contractors are invited to participate in a non-competitive Walk/Fun Run.
Clinical Center Grand Rounds Lecture
Gene-Forecast: The Systems Biology of Cardiovascular Health Disparities; Tailoring Mobile Health Technology to Improve Cardiometabolic Health in Resource-Limited Neighborhood Environments: A Multi-Level, Community- Based Approach
June 17, 2015, Noon – 1:00 p.m.
Lipsett Amphitheater
Presented by Gary H. Gibbons, MD, NHLBI and Tiffany M. Powell-Wiley, MD, MPH, NHLBI.
The Children's Inn at NIH: 25th Anniversary Symposium[disclaimer]
At the Intersection of Hope & Science: 25 Years of Advancing Medical Discoveries
June 18, 2015, 2:00 p.m. – 5:30 p.m.
Masur Auditorium
The symposium will highlight The Inn's history and role in advancing medical research. NIH physicians and families will share their stories and the fascinating scientific advances that have been made in treatment of their diseases.
NOTE: PDF documents require the free Adobe Reader.
 The information on this page is archived and provided for reference purposes only.
The information on this page is archived and provided for reference purposes only.

