Clinical Center News
CC chef participates in "Chefs Move to Schools" campaign
 |
|
CC executive chef Robert Hedetniemi turns up the heat in a demonstration for Nutrition Department staff members Janet Hoey (left) and Christina Johnson.
|
By: Nicole Martino
There are two ways to get kids to eat healthy food, says Robert Hedetniemi, certified executive chef for the Clinical Center's Nutrition Department—you can trick them or you can teach them.
"It's tough to get kids to eat stuff they aren't accustomed to. The way I see it, you can either hide it in things that they like, or you can get them involved in the cooking process," he said.
Hedetniemi has recently joined the ranks of individuals and organizations supporting First Lady Michelle Obama's Lets Move! campaign to solve the childhood obesity epidemic within a generation. He is one of hundreds of chefs from across the country who have signed up to be part of the "Chefs Move to Schools" initiative, a program that pairs chefs with community schools to help teach young people about nutrition.
Run through the US Department of Agriculture, "Chefs Move to Schools" asks culinary professionals to create healthy meals that meet the schools' dietary guidelines and budgets. The chefs and schools—kindergarten through grade 12—will also work together to teach young people about nutrition and making balanced and healthy choices. Hedetniemi has not been paired with a school yet, but left the June 4 kickoff event on the White House lawn feeling inspired and excited.
In her opening remarks at the kickoff rally, First Lady Michelle Obama explained the severity of the problems associated with childhood obesity. "You all know the statistics when it comes to the health of our kids—and they're staggering, every time we talk about it—how nearly one-third of children in this country are now overweight or obese. That's one in three. Just think about that. That means that these kids are at greater risk of obesity-related diseases—you name them, cancer, heart disease, stroke," she said.
Hedetniemi agrees. "If we don't do something about it now, we are going to have a generation of kids with extreme health problems who are going to grow up into adults with extreme health problems," he said. "We have an opportunity now to intervene, and from my little role I think I can expose some kids to some really cool products to help them get excited about nutrition."
As a dad to four kids, Hedetniemi has seen what school lunches look like, and as a former restaurant owner, he understands the financial pressure school food programs can experience.
 |
|
Robert Hedetniemi of the CC Nutrition Department has joined the White House "Chefs Move to Schools" initiative to teach children how to make healthy choices.
|
"Schools are under a budget and I understand that, but I believe that a better job can be done," he said.
Hedetniemi says he got addicted to cooking at the age of 13 after he took his first job in a restaurant. After serving four years in the Navy, he studied culinary arts at Johnson & Wales University in Rhode Island. Prior to joining the NIH, Hedetniemi owned three businesses outside of Hilton Head, SC. He joined the Nutrition Department in December 2009.
At the CC, Hedetniemi creates weekly specials for inpatients and uses his culinary experience to produce diverse menu items from scratch. He is also an important resource for other nutrition staff members who have questions about food preparation or production, especially for patients with special dietary needs or requests.
"The mission of the NIH really excites me, and I can utilize my skills to help a cause that I really believe in—eradicating disease," he said.
Another cause Hedetniemi believes in is educating children on the good taste and benefits of healthy food, and he thinks he can make a real difference in that arena. The executive chef pointed out that the Food Network and other television shows have made chefs into celebrities whom kids look up to. Another set of role models who influence children's behaviors is parents, Hedetniemi said.
"Kids can only make decisions based on what they have been exposed to. As a parent, if you want to get better products into your children, expose them to as much quality food as possible," he said.
Back to Top
First full genome sequence completed on NIH patient
The first NIH patient to have his whole genome sequenced calls the experience "fabulous" and "eye-opening."
Rick Del Sontro was first to have researchers complete a detailed description of the order of the chemical building blocks, or bases, in his DNA. As part of the National Human Genome Research Institute (NHGRI)'s ClinSeq™ study, this milestone advances toward personalized medicine and a better understanding of how patients may react to their genetic information.
"Ultimately what personal genomics is all about is finding out what your risks are and modifying your behavior accordingly to maximize staying healthy," NIH Director Dr. Francis S. Collins told science reporters in May.
The ClinSeq™ study is a trans-NIH effort to understand the genetic roots of disease susceptibility and the challenges of using genome (the entire set of genetic instructions found in a cell) sequencing tools in a clinical research setting. It is also the first study to return individual genetic sequencing results to research subjects from a large-scale sequencing effort. Coronary heart disease is a good place to start because of its high association with genetic risk factors and the numerous interventions available, reported the research team.
While most ClinSeq™ participants were initially sequenced for about 300 genes known or suspected to be associated with heart disease, Del Sontro was the first chosen for whole genome sequencing. In this process, a person's three billion base pairs are sequenced to identify the million or so variants that make everyone unique and hopefully link some of those to risk of disease. Patients want to know, "What's wrong with me? What caused it? What can we do?" said ClinSeq™ principal investigator Dr. Leslie Biesecker, chief of the NHGRI Genetic Disease Research Branch. "We want to use these genomic technologies to answer those embarrassingly simple, but difficult, questions."
Del Sontro enrolled through a referral from the NIH Heart Center at Suburban Hospital in Bethesda, Md. With a family history of heart problems, he forced himself on a cardiologist, even though he appeared in good health with an Ironman triathlon to his record. His doctors found "off-the-charts calcification," of his coronary arteries Del Sontro said, and, after treatment, recommended him to the ClinSeq™ study for further investigation of an underlying cause.
Launched in 2007, the research protocol invites participants to the Clinical Center for a half-day clinical work-up that includes visits to phlebotomy and the EKG heart station. A partner in the study, the National Heart, Lung, and Blood Institute performs an echocardiogram and a computerized axial tomography, or CAT, scan of the heart on each ClinSeq™ patient volunteer.
"We get a snapshot of the current state of that person's heart health," Biesecker said. "We can use that as the starting point, but only as the starting point, to begin to dissect their long-term risk of having heart disease."
The blood participants donate is screened for markers like cholesterol and glucose levels, and some is sent to the NIH Intramural Sequencing Center where the 300 candidate genes or, in Del Sontro's case, the whole genome is sequenced.
He was selected for the more comprehensive sequencing because of the unusual presentation of plaque buildup in his arteries but no history of high cholesterol, said genetic counselor and ClinSeq™ researcher Flavia Facio. Del Sontro shares this unique health history with generations of his family and his seven brothers and sisters. Many of them have joined the ClinSeq™ study. While the initial analysis of Del Sontro's genome has not yet revealed the genetic mutation that causes his hereditary heart disease, it did show that he has inherited a condition called hereditary neuropathy with liability to pressure palsies, which causes numbness in his extremities.
Though there is no cure, he said he is glad to have an explanation for the trait. Such knowledge could be comforting after symptoms have arisen, but it is still unclear if patients want to know about their odds of future disease. Another goal of the ClinSeq™ study is to assess how patients feel about genome analysis, which might reveal risk for serious conditions.
"We want to know what patients want; what patients think; what they'll do with the data," Facio said.
She discusses with study participants the possible outcomes and what results they would like to be notified of. Her anecdotal experience is that most want to know what their tests and gene analysis reports, but Facio is careful to note that her study population is self-selected and not generalizable.
She reports that another patient has been selected for whole genome sequencing and that others are undergoing exome sequencing (just the portions of genes that code for proteins, thought to contain most mutations that have a major effect on the cause or predisposition to diseases).
"We are intrigued about insights we are gaining from the study so far," Biesecker said. "I think the research will be driven by collaboration and what we find in the sequencing."
Back to Top
Movement Analysis Lab steps into renovated space with latest equipment
More tools make for better research in the Clinical Movement Analysis Lab (CMAL) in the Clinical Center Rehabilitation Medicine Department Functional & Applied Biomechanics Section (FABS). A recently renovated space brings the latest in motion capture and analysis equipment to the study of how patient populations move.
After two months displaced to the Medical Arts television studio on the B2 level, the team moved back into their lab in the Rehabilitation Medicine Department in February. The renovations were funded by the phenotyping core of the Center for Neuroscience and Regenerative Medicine. Tasked with learning more about traumatic brain injury to develop treatments and therapies, the center is a collaboration between the NIH, the Uniformed Services University, the Walter Reed Army Medical Center, the National Naval Medical Center, and The Henry M. Jackson Foundation for the Advancement of Military Medicine.
 |
|
The Clinical Movement Analysis Lab captures patients'—like Joshua Watson, 11, who has cerebral palsy—gaits with markers and cameras and displays the movement in real-time on a screen in the room.
|
Eventually CMAL staff will see traumatic brain injury patients and help in the categorization and study of pathogenesis for those with such conditions.
The CMAL uses a combination of tools—cameras, electrodes, force plates, and a new body weight support system—to give a comprehensive view of how patients with debilitating disorders such as cerebral palsy and osteogenesis imperfecta move. While the focus is on walking, any type of movement in any part of the body can be measured.
"Combining all those data gives a full quantitative analysis," said Lindsey Bellini, an FABS engineer. The goal is to develop new strategies to improve movement and to test those strategies already in place, said Chris Stanley, senior research engineer in the FABS.
The primary piece of the puzzle involves ten new cameras that measure motion—improved from seven older cameras—by recording the changing positions of reflective markers on specific locations of the patient's body. A bone model created from the reflective markers calculates joint angles, for example how much the knee bends when walking. The new motion-capture system features real-time capability, where the software processes the motion as it occurs, rather than after the motion is completed. This allows for more advanced studies and lets researchers check that the capture technology is set correctly and adjust if necessary. Tiny, wireless electromyography electrodes are time-synchronized with the system and measure muscle activity, such as when they fire to propel the person.
"Plus it's really cool to show people, 'this is what you're doing right now,'" Bellini said of the technology also used in sports performance analysis and motion picture technology.
A color pattern on the floor camouflages plates that measure three dimensional forces and moments in each patient's step. With a lot of pediatric visitors, the colors are also "just more fun for the kids," Stanley said.
A bigger, better treadmill also holds force plates. The treadmill is split, right and left, to measure and compare forces on each side. The treadmill will be used with a new virtual reality system that will be tested first in patients with Parkinson's disease or traumatic brain injury, the engineers said. This type of system can 'trick' the person to step over obstacles or navigate through a narrow hallway or busy store, to more realistically assess how they function in everyday life.
The last piece to be installed was a body weight support system with a track extended over the force plates and treadmill. The patient wears a harness that is connected to the system, allowing the team to provide support to enable weak or heavy patients to practice walking when they would not be able to on their own. Additionally, the support system can help patients safely practice more difficult tasks, such as running or deep squats, without a fear of falling. The support is dynamic, that is the same tension is held through the entire exercise, both when pulling away and when moving closer through the natural gait pattern.
"This allows us to start rehabilitation sooner and accelerate people more quickly. When they're not supporting their entire body weight, they can challenge themselves," said Bellini.
Data from all the CMAL tools are combined to form a more complete picture for both patients with motor disabilities and healthy volunteers (for comparison sake). The lab measures the effects of interventions—everything from surgery to medications, a brace to an exercise regime—to see if the patient makes and retains progress. For example, the movement of a young child with a brain injury would be captured and analyzed before, during, and after completing an exercise program on the elliptical machine to see if greater practice of making reciprocal arm and leg movements would translate to faster and better walking.
Back to Top
BTRIS leader updates on research information system year after launch
 |
|
Dr. Jim Cimino demonstrated the sorting capabilities of BTRIS to a group of NINDS intramural researchers in June.
|
Dr. Jim Cimino, chief of the Clinical Center Laboratory for Informatics Development, gave an update on and demonstration of the Biomedical Translational Research Information System (BTRIS) on June 22.
"BTRIS is designed to bring together clinical research data from all the institutes and centers to give investigators one place to get all their data and allow other users to ask new questions of the old data," Cimino said.
The system, launched July 2009, is available to the NIH intramural community and brings together clinical research data from the CC and other institutes and centers. BTRIS provides clinical investigators with access to identifiable data for the subjects on their own active protocols, while providing all NIH investigators with access to de-identified data across all protocols. The advanced search, filtering, and aggregation methods to create data sets support ongoing studies and stimulate ideas for new research.
Last month's audience from the National Institute of Neurological Disorders and Stroke had questions on time lapse of data availability and informed consent. Cimino reported that new entries into the Clinical Research Information System (CRIS) can be seen in BTRIS two days later. His system is not intended for patient care, he reminded, and CRIS should be the first stop for current patients' information.
Regarding permission to view data from other investigators' protocols, Cimino assured that the NIH Office of Human Subjects Research has approved the appropriate, monitored use of de-identified data by other researchers.
His demonstration included an example of BTRIS' utility. After noticing that average albumin levels were dropping in all patients, Cimino sorted those lab results according to year and found that mean albumin decreased steadily while standard deviation remained constant. He plans to pursue this pattern in a future research protocol.
With use and interest from the NIH community climbing, the BTRIS team hopes to streamline the notification process (investigators must approve use of their de-identified data, even on closed trials if they are less than five years old) and add data from more institutes and centers.
For more information, visit http://btris.nih.gov.
Back to Top
Decker Lecture combats myths around hospital-acquired infections
 |
|
Dr. Tara Palmore presented the 2010 John Laws Decker Memorial Lecture on "Hospital Infections: Rumors and Reality."
|
The seventh in a series honoring NIH leaders in clinical teaching, the 2010 John Laws Decker Memorial Lecture on June 9 highlighted the work of Dr. Tara Palmore, deputy hospital epidemiologist at the Clinical Center and staff clinician at the National Institute of Allergy and Infectious Diseases. Palmore is the recipient of the NIH Fellows Committee's 2009 Distinguished Clinical Teacher Award.
Palmore's lecture, "Hospital Infections: Rumors and Reality," addressed common misconceptions about hospital-acquired infections, an area of interest of the NIH community evidenced by the crowd at Lipsett Amphitheater.
The annual lecture is presented in memory of former CC Director Dr. John Laws Decker, who died in 2000. He served as director of the CC and as NIH associate director for clinical care from 1983 until 1990, after which he was named scientist emeritus. Decker's children, Dr. Megan Molaro and David Decker, and his grandson Ian attended the lecture.
Palmore came to the NIH in 2001 as an infectious disease fellow after completing her medical degree at the University of Virginia School of Medicine and residency at New York-Presbyterian/Weill Cornell Medical Center. She joined the NIH staff in 2005 and became deputy hospital epidemiologist in 2007. Palmore directs development, organization, and implementation of the CC infection control program.
Hospital-acquired infections—which affect 1.7 to 2 million people a year and kill an estimated 99,000—come at a serious cost, economically and socially, Palmore said.
"An intangible but extremely important consequence of hospital infections is a loss of public confidence in the health-care system, which allows these infections to occur in a place where people go to get well," she said.
 |
|
On June 9 the family of Dr. John Laws Decker celebrated the naming of a guest room at the Edmond J. Safra Family Lodge in honor of the former CC director in appreciation of a donation to the lodge through the Foundation for NIH. Present to note the occasion were (from left) Decker's son-in-law James Malaro; Decker's son David Decker, his wife Lisa Greenlees, and their son Ian; CC Director Dr. John I. Gallin; and Decker's daughter Dr. Megan Malaro.
|
Palmore refuted the misconception that "hospital infections are bound to happen" and explained ways health-care professionals can prevent and treat infections. Palmore discussed the CC policy of mandatory flu vaccination for patient-care staff.
"The reality is that flu vaccination of health-care workers saves patient lives," she said.
Palmore discussed strategies to prevent or terminate the transmission of infection and encouraged lecture attendees to always consider the possibility of an outbreak until proven otherwise, that is to avoid viewing single infections as isolated incidents or coincidences.
"Hospital infections should not be accepted as a normal part of patient care," she said. "We aren't going to get certificates for having clean hands, but preventing infections is really its own reward."
A videocast of Palmore's lecture is available in the Grand Rounds archives at http://videocast.nih.gov.
Back to Top
Unique CRTP student helps spread CC mission
Clinical Research Training Program (CRTP) fellows exhibited the products of their 12-month tenure at the NIH with poster and oral presentations of their research projects during May's NIH Spring Research Festival and the annual CRTP Scientific Presentations. This year's CRTP class was fortunate to include a new kind of medical student.
The CRTP, under the direction of the Clinical Center Office of Clinical Research Training and Medical Education, is a public-private partnership supported jointly by the NIH and a grant to the Foundation for NIH by Pfizer Inc. Medical and dental students spend a year engaged in a mentored clinical or translational research project in an area that matches their personal interests and goals.
Jeremy Forcé is the first CRTP fellow from an osteopathic school of medicine. While the medical training is exactly the same as allopathic (Western) medicine, there are subtle differences that are more philosophical than anything else, Forcé explained.
"Osteopathic medicine looks at a specific disease in the context of the body as a whole. Most allopathic physicians inherently take this whole body approach, so today there really are not many differences," Forcé said.
 |
|
Jeremy Forcé presented on his CRTP research project on May 17. During his year at NIH, Forcé looked at outcomes from various measurement criteria in treated cancer patients to retrospectively determine how these criteria would have affected clinical management.
|
Forcé presented in May on "Volumetric Analysis of Lung and Thymic Malignancies: Clinical Implications," a retrospective evaluation of clinical outcomes based on different measurement criteria used in treated thymic cancer patients. A student at the University of New England College of Osteopathic Medicine, Forcé worked under the guidance of Dr. Giuseppe Giaccone, chief of the Medical Oncology Branch of the National Cancer Institute. "The program in and of itself has been a tremendous experience. My ability to network throughout the NCI, be involved with writing protocols, see patients on clinical research studies, and be able to perform other types of clinical research has opened my eyes tremendously," Forcé said.
Forcé learned about the CRTP as co-president of his college's research club and has presented on the opportunity to his classmates. "I have already had multiple students who responded and have said they are either considering or going to apply to CRTP," Forcé said.
According to the American Association of the Colleges of Osteopathic Medicine, nearly one in five US medical students is training to be an osteopathic physician. Still, because of osteopathic medicine's focus on primary care, there are few osteopathic medical students in academic and institutional research.
In the future, Forcé hopes to see more osteopathic medical students pursue research avenues. "It would be a true hope of mine to see more students in this program or others like it," he said.
Back to Top
Former patient celebrates life after beating cancer at the NIH
 |
Robert Longo spoke on the 35th anniversary of his cancer diagnosis, a disease he beat at the NIH in 1978.
|
Robert Longo celebrated an anniversary in June. Given a 20 percent chance of living two years, Longo has survived 35 years after a bone cancer diagnosis at age 15.
He was diagnosed on June 10, 1975, a date his mother, Margaret, rattles off from memory easily. Living in Rockville at the time, Longo learned of an NIH protocol for the cancer that would take his left leg above the knee.
The others in the study were also teenagers. "They did two legged races down the hall and drove the nurses wild," Margaret said.
Nurses organized a wheelchair basketball game to amuse the teens in the days before video games and VCRs. Longo fell from his chair and had to have surgery.
"I was made acutely aware of the need for blood," he said.
That realization inspired his project to earn "life rank" in the Boy Scouts of America: a blood drive at the NIH Blood Bank where more than 100 people donated 92 pints of blood. Longo went on to organize another blood drive at the NIH and continues with the practice.
Spring 1978 marked his last chemotherapy appointment, and Longo graduated high school soon after to a standing ovation. He credits his attitude with helping him survive—treatment was one part of his life and school was another. He kept his two worlds separate, Longo said.
"He never acted like a victim," Margaret said.
Longo has worked as a salesman, but is affected by scoliosis—curvature of the spine. He lives in Germantown and continues a relationship with the CC. Longo donates books to the patient library and wrote a letter advocating expansion of the space.
He celebrated his 35th year since his cancer diagnosis with a celebration at his church on June 13.
Back to Top
2010 Medicine for the Public looks at heart health
 |
|
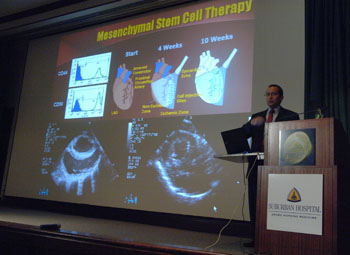
Dr. Keith Horvath of NHLBI spoke at the 2010 Medicine for the Public lecture on May 25.
|
Dr. Keith Horvath intrigued audience members with a vivid, real-time graphic presentation on the future of cardiac surgery during the 2010 Medicine for the Public (MFP) lecture on May 25 at Suburban Hospital in Bethesda.
Horvath is director of cardiothoracic surgery at the NIH Heart Center at Suburban Hospital and director of the Cardiothoracic Surgery Research Program at the National Heart, Lung, and Blood Institute (NHLBI).
Also presenting on the emerging science of epigenetics and its influence on heart health and disease was Dr. Dina Paltoo, chair of the NHLBI Data Access Committee and program director of the NHLBI Advanced Technologies and Surgery Branch in the Division of Cardiovascular Diseases.
Clinical Center Director Dr. John I. Gallin opened the lecture recognizing the MFP's new collaboration with Suburban Hospital and Johns Hopkins Medicine, coupling the strengths of the three institutions for an enhanced health education experience.
The lecture is available on videocast at the MFP website www.cc.nih.gov/about/news/mfp.shtml.
Back to Top
Helping high school scientists reach international fair
By: Nicole Martino
 |
|
Aditya Mazmudar enlisted the help of the CC Department of Laboratory Medicine on the project that won him and his partner a prize at the Intel International Science and Engineering Fair.
|
Over the past several months, Nayana Patel has helped two important things grow: young scientists and bacteria.
Patel is a supervisor in the bacteriology section of the Clinical Center Department of Laboratory Medicine (DLM) Microbiology Service. She worked with two Fairfax High School students on their science fair project entitled "A Novel Gallium/Zinc Nitrate-Based Intravenous Medicine for the Treatment of P. Aeruginosa Nosocomial Infections".
"Working at NIH was an unparalleled opportunity and experience for both of us," said Aditya Mazmudar, who, along with partner Atif Javed, spent several Saturdays in the DLM with guidance and supervision from Patel. "We got to use a wide variety of instruments and actually experience what it was like to be a researcher," Mazmudar said.
Mazmudar and Javed's project sought to employ a gallium and zinc (chemical elements) nitrate-based substance to kill the bacterium Pseudomonas aeruginosa. They researched and designed the project independently and came to Patel for instruction on using the appropriate materials and for the laboratory space itself.
"It is the most fun to teach them the technical part, and also I get to learn some new stuff," Patel said.
The project won Mazmudar and Javed grand prize at the Fairfax High School science fair and at the Fairfax regional science fair. In May, the team went on to participate in the Intel International Science and Engineering Fair in San Jose, Calif., where their project placed fourth in the health and medicine category and received recognition from the US Naval Research Laboratory and the American Association of Pharmaceutical Scientists.
Mazmudar describes Patel as an extremely knowledgeable and irreplaceable mentor. "She really refined our research project and procedure," he said.
Patel, who has been involved in science fair projects before, said that she was glad she could help and is proud of the team for their accomplishments. "It is important to help young kids, especially those interested in science, grow and learn new things."
Back to Top
Research leader presents on Haiti after earthquake
Things were tough in Haiti before the January earthquake, but Dr. Jean "Bill" Pape's team was making a difference. They are continuing to do so as the nation recovers from the natural disaster.
Pape shared his experiences as director of GHESKIO in Port-au-Prince, Haiti, the first institution in the world dedicated to the fight against HIV/AIDS, and the state of the country he has served since 1979 in "Report from Haiti: Rebuilding Research & Training Programs in the Aftermath of Disaster" in Masur Auditorium on June 17.
NIH Fogarty International Center Director Dr. Roger I. Glass said Pape, an NIH grantee, "has made an incredible contribution to health in Haiti."
GHESKIO has provided continuous medical care since 1982 when the organization grew out of efforts to curb infant diarrhea. Pape's team was asked to look at adult cases that turned out to be among the first cases of HIV/AIDS. Additionally, GHESKIO does research into treatment for congenital syphilis and tuberculosis.
Pape showed photos of his staff, some who have been with him from the beginning. "It is people who make an institution," he said.
The organization lost four staff members in the earthquake, but GHESKIO has held a presence through the turmoil. They set up an acute care field hospital with the US Department of Health and Human Services and a tent city for the hundreds of thousands without shelter.
Enrollment and training were halted immediately after the earthquake but the programs for new lab technicians, nurses, physicians, and community members have resumed. GHESKIO also runs a nurse practitioner training program and supports a master of public health degree program at a local university.
"Synergism between research training and clinical care can have an impact even in a disaster," said Pape.
Back to Top
Atrium hosts NIH Philharmonia
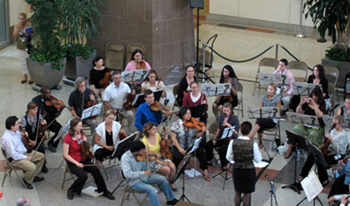 |
Photo by Dr. Francoise Meylan
|
The NIH Philharmonia performed under the direction of Dr. Nancia D'Alimonte in the Clinical Center atrium on June 15.
The all-volunteer orchestra was founded at the National Institutes of Health in January 2005 under the professional musical direction of D'Alimonte.
The CC performance featured selections from Vivaldi and Mozart. Emile Gogineni, a post baccalaureate student training in the CC Critical Care Medicine Department, played a violin solo in "Summer" from Vivaldi's Four Seasons.
For more information about the orchestra, visit http://www.nihphil.org
Back to Top
Patient granted US citizenship in CC ceremony
To the tune of Woody Guthrie's "This Land is Your Land," Clinical Center patient Hariam Taye swore an oath of allegiance to the United States in an April citizenship ceremony held especially for her on the 3NE inpatient unit. Jacob Djaboury, a supervisory immigration services officer, administered the oath.
"I am so glad that I had the opportunity to come here. I understand how important a ceremony like this can be," he said.
Taye was unable to attend previous immigration ceremonies due to illness, but expressed her sincere gratitude to the small crowd of doctors, nurses, and social workers who attended the event. The group celebrated with red, white, and blue cake and American flags distributed by Djaboury.
Back to Top
Oncology nursing goes west
The 35th Oncology Nursing Society Congress was held May 13—16 in San Diego, and four NIH representatives attended. Geoffrey Seidel of the National Cancer Institute, Michelle Eugeni of Clinical Center Nursing and Patient Care Services, Judy Smith of the NCI Division of Cancer Prevention, and Maureen George of the CC Department of Anesthesia and Surgical Services had the chance to connect to more than 4,000 of their peers. Though each in a different clinical area at NIH, they all benefited from hearing the most cutting-edge educational offerings, including a presentation on nanotechnology that Seidel gave.
The Oncology Nursing Society Foundation—funding local and national oncology nursing education, research, and leadership opportunities—promoted a balanced work life by holding its annual 5K run. Smith and George participated and said they found great satisfaction in their "timely" completion.
Back to Top
Team NIH races to support breast cancer research
Members of the NIH community—staff from across institutes and centers and their families—banded to form Team NIH at the Susan G. Komen Global Race for the Cure on the National Mall in Washington, DC, on June 5.
The five-kilometer race raised money for breast cancer research and united survivors and activists.
Back to Top
Consider becoming a CFC keyworker
The Clinical Center Combined Federal Campaign (CFC) committee is looking ahead to another successful season of raising funds for those in need. Consider becoming a CFC keyworker and taking a more active role in the campaign.
Keyworkers are the link between the CC CFC committee and employees. Motivate your peers to give what they can—participation is the main goal—and answer questions. The CC CFC committee is always available for support.
In addition to helping make a real difference to the various charities that rely on the CFC, keyworkers gain access to months of can't-miss activities. Exclusive events with food, fun, and friendly faces await the 2010 CC CFC keyworkers.
Speak to your department head about taking on this new role.
Back to Top
This page last updated on 12/18/2017


 The information on this page is archived and provided for reference purposes only.
The information on this page is archived and provided for reference purposes only.