Clinical Center News
Ambassadors color the CC with dedication
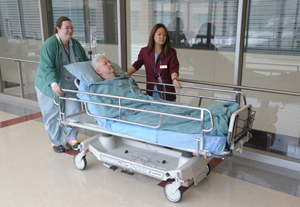 |
Supervisory health technologist B.B. Holstein (left) practices patient transfer with ambassador Cynthia Kim and Ben Abad, another health technologist, between the surgery and intensive care units.
|
Staff, patients, and visitors are used to white coats filling the halls of the Clinical Center, but a new color has joined the ranks. The patient ambassador program, launched October 1, has outfitted a band of 65 volunteers in burgundy jackets to reduce CC spending and increase visibility of those who donate their time to the NIH.
Tasked with reducing the cost of the messenger and escort contract by extracting duties that volunteers could perform, a task force led by Denise Ford, CC Hospitality Services, and Courtney Duncan, CC Volunteer Services, devised a plan to find and train a competent team. Recruitment efforts, including phone calls and mailings to local organizations, online outreach, and open houses, brought in an initial group of 70 patient ambassadors.
More than just cutting spending, the patient ambassador program strengthens community relations and fosters inclusion and diversity. The group includes Intramural Research Training Award recipients, staff scientists, retirees, high school students, and the disabled. The program has ambassadors handling patient transport in Radiology and Imaging Sciences and the Department of Anesthesia and Surgical Services, medical record transport, and wheelchair management. Volunteers are asked to commit a minimum of four hours of service a week for one year.
Cynthia Kim works in the surgery department transporting patients, helping as she can and learning the ropes. The Montgomery College student would like to eventually be a surgeon and enjoys the patient contact of the ambassador program.
Patient ambassador liaison, B.B. Holstein, supervisory health technologist, is grateful for Kim and the other 15 ambassadors who help around the operating room. “Volunteers generally want to be here, and that shows,” Holstein said.
The ambassadors and the department have a symbiotic relationship, Holstein said. She tries to familiarize them with the surgical environment while they provide a service. “They’re getting experience. We’re getting help.”
Patients, too, seem impressed by their new caregivers’ service and dedication. “The patient ambassadors are so warm and caring. They take time with you,” one shared about the new program.
“You all have made this program very visible, and the enormous success is directly attributable to you, your caring personalities and genuine will to contribute,” Ford wrote in an e-mail to ambassadors celebrating the program’s six-week mark.
Recently welcoming seven more ambassadors, the program is continuing recruitment with sights set on expanding into more CC departments.
Back to Top
Mind, Body, Soul
Staff complete integrative medicine fellowship
 |
|
Drs. Jay Shah and Gwenyth Wallen completed an integrative medicine fellowship in December, sponsored by the Bravewell Collaborative, through the Univeristy of Arlzona medical school.
|
Two Clinical Center employees recently completed the prestigious two-year Bravewell Associate Fellowship Program in Integrative Medicine.
Dr. Gwenyth Wallen, chief of the research and practice development service in Nursing and Patient Care Services, and Dr. Jay Shah, senior staff physiatrist in the CC’s Rehabilitation Medicine Department, graduated December 12 from the program, offered through the University of Arizona medical school’s program in integrative medicine (PIM).
The comprehensive program includes 1,000 hours of instruction in biologically based therapies (phytochemicals, supplements, and botanicals), mind-body therapies (breath-work, progressive muscle relaxation, and meditation), manual medicine (massage therapy, osteopathy), and spirituality and energy medicine (qigong, reiki), among others. Various whole system therapies are also presented, including homeopathy, traditional Chinese medicine, and Ayurvedic medicine.
Fellows also complete three residential weeks in Tucson. Curriculum presented via the Internet—videos, e-mails, and online discussions—allowed fellows to participate from across the nation.
In addition to these studies, the Bravewell Collaborative also provided Shah and Wallen with the opportunity to complete clinical rotations at one of the eight leading clinical centers comprising the Bravewell Clinical Network.
The Bravewell Collaborative is a community of philanthropists dedicated to advancing integrative medicine through the funding of research initiatives and collaboration with like-minded physicians and organizations. It emphasizes healing that focuses on the entire person—body, spirit, mind, and community.
The first class of Bravewell-sponsored fellows enrolled in the program in January 2005. The program proved effective in furthering the collaborative’s mission, and a second class of 23, including Wallen and Shah, began their training in January 2007.
Wallen was approached by Dr. David Henderson, CC deputy director for clinical care, to apply for the fellowship because her research entails integrative medicine. Wallen is studying the health behaviors of Hispanic and African-American patients with rheumatic diseases, including their use of complementary and alternative treatments. She is also conducting a randomized, controlled clinical trial exploring the use of hypnosis as a pain and symptom-management strategy for the treatment of sickle-cell disease patients.
In her clinical rotation at The Penny George Institute for Health and Healing at Abbott Northwestern Hospital, Minneapolis, Wallen attended inpatient rounds and shared her current and future research plans with the interdisciplinary integrative health team. Feedback she received included the suggestion for a renewed focus on the relationship between an individual’s susceptibility to hypnosis and biomarkers such as nitric oxide and Vitamin D levels.
“The fellowship has been great for me both personally and professionally because it honed my knowledge and skills in integrative medicine. I’ve been able to share my research and just the idea of doing this kind of research,” Wallen said.
Shah echoed the sentiment, noting that complementary and alternative approaches too often rely on anecdotal evidence. “[This] is an excellent program because it emphasizes the importance of scientific evidence-based integrative approaches wherever possible.” He also enjoyed the opportunity to present his research and to encourage research among his peers.
The Bravewell Fellowship, together with his clinical rotation at the University of California, San Francisco’s Osher Center for Integrative Medicine, reaffirmed for Shah the importance of integrating the bio-psycho-social aspects of health care with modern science to provide optimal patient care.
Shah and his colleagues are studying the biochemical milieu of myofascial trigger points—discreet, palpable, hyperirritable nodules in taut bands of skeletal muscle. He commonly treats myofascial pain with dry needling, a form of mechanical myofascial release with the goals of reducing abnormal muscle contractures, relieving pain, and restoring range of motion and function. Although he uses acupuncture needles, Shah emphasizes that dry needling is quite different from traditional acupuncture—a practice from ancient China based on the flow of energy through acupuncture meridians. He teaches dry needling and other treatment techniques through Harvard Medical School’s “Structural Acupuncture for Physicians” course.
For more information on Shah’s research, see the May 2008 issue of CC News online at http://www.cc.nih.gov/about/news/newsletter/2008/may08/newsletter.html#4.
Back to Top
Therapy program offers release and support for patient families
 |
|
Using toy sets to simulate medical procedures helps patients’ children like 3-year-old Sydnie Gapper from Oregon become comfortable with their parent’s treatment. Sydnie listens to her bear’s heart with a toy stethescope as her mother Grace (middle) and Recreation Therapy Chief Donna Gregory look on.
|
Braydon Philpot, 11, boasts of his video game records and works on a construction-paper turkey in the Clinical Center main playroom a few days before Thanksgiving.
“I’ve jumped that finish line three times,” he says as his hands cut and glue. He’ll be home in Lancaster, Pa., for the holiday, and can’t wait to see his dog, Philpot excitedly tells the playroom therapists. A frequent visitor, Philpot and his parents are thankful to the Family-Centered Care Program (FCCP) of the Rehabilitation Medicine Department’s Recreation Therapy Section for the release from the stress of care.
Diagnosis and treatment of a life-threatening illness is a strain on the family unit. Children are forced to address mature subjects, and parents are distracted with quality-of-life decisions. The Family-Centered Care Program offers programs and support to allow family members to re-inhabit their traditional roles—parents bake cookies with daughters, children eat pizza and attend sing-alongs with their peers.
The program specifically addresses the unique needs of children of adult patients and siblings of pediatric patients. “The FCCP involves activities to encourage participants to talk about their feelings and talk about medical issues in an age-appropriate, kid-centered way, and offers a place and time to just be a kid amongst the chaotic, unfamiliar world of NIH,” said Recreation Therapy Chief Donna Gregory.
 |
James Galvin (left) joins the Hewitt family—Kathryn (second from left), Katie and Joel—from West Virginia at the Family-Centered Care Program’s cookie decorating event on November 19 in the main playroom.
|
The program began in May 2008 to provide direct support for the families of patients. “We hope it will contribute to compliance—people will stay here, stay in protocols—if their family is cared for,” said recreation therapist Karen Perkins. The program sponsors events about twice a week and hopes to integrate more inter-generational activities, Perkins said. Children or siblings of patients are also welcome to drop in to the main playroom between 10 am-12 noon and 1 pm-3 pm.
“The program creates alliances in families, either those here for the same treatment or from the same part of the county. It creates support networks,” said Perkins. Philpot found an ally in a girl whose father is fighting the same battle his is: chronic lymphocytic leukemia.
To help the children better understand what their sick family member is going through and to allow them to ask questions, the recreation therapists use books, structured therapeutic activities, and interactive medical play games.
For some the reasons for attending Family-Centered Care Program events are not as complex as coping or support. Asked why he attended a cookie decorating party on November 19 with his mother and sister, patient Joel Hewitt, 22, responded, “I love cookies.”
Back to Top
Former NIH nurses, Fauci honored with medical movie awards
 |
|
Rear Adm. Carol Romano, assistant surgeon general (left), presented Vernice D. Ferguson (right) with the 2008 Lifetime Achievement Award.
|
And the FREDDIE goes to …
Two former Clinical Center nurses and NIAID Director Dr. Anthony S. Fauci were among those recently honored at the 34th Annual FREDDIE Awards presented by the MediMedia Foundation to recognize excellence in electronic, health-related educational materials.
Former chief of the Nursing Department Vernice D. Ferguson was given the 2008 Lifetime Achievement Award at the November 13 event held in Philadelphia. Fauci received the 2008 Public Service Award for his outstanding contributions to the infectious disease field.
The FREDDIE Awards take their name from Dr. Fred Gottlieb, a San Francisco Bay Area ophthalmologist who was inspired to join the field of medical film production and launch a competition for such work after viewing a particularly dull surgical film. The MediMedia Foundation carries on his work to acknowledge and encourage filmmakers, thereby advancing the art, promoting social welfare, and furthering the education of medical professionals and health consumers.
The 2008 Lifetime Achievement Award was presented to Ferguson by Rear Adm. Carol Romano, assistant surgeon general, chief nurse officer in the US Public Health Service, and senior advisor in the CC’s Department of Clinical Research Informatics. Ferguson is senior fellow emeritus in the School of Nursing at the University of Pennsylvania. She served for 12 years as the assistant chief medical director for nursing programs in the Department of Veterans Affairs after heading the CC’s Nursing Department from 1972 to 1980.
The ceremony’s program literature praised Ferguson, “She has accomplished so many ‘firsts’ as an African-American, as a woman, and as a nurse that she stands in a league of her very own.”
Another former NIH nurse was honored for her numerous leadership roles with the FREDDIE Awards over the course of 24 years. Donna Hill Howes served as executive producer of the event and president of Staywell Productions and is vice president of the board of directors of the MediMedia Foundation. She worked as a nurse for NCI, NICHD, and NEI during her NIH tenure from 1970 to 1982.
Hill Howes is passing on her producer post and leaving Staywell for a position with the Bill & Melinda Gates Foundation, but is overjoyed that she was around to see Ferguson recognized. “I have always nominated a nurse. It is just magic that the last year I am at the helm they honor a nurse,” she said.
The FREDDIE Awards’ 2008 Public Service Award winner Fauci was touted as “the public face of AIDS research and efforts to combat bioterror.” Previous recipients of the same award include Dr. Vincent T. DeVita, Jr.; Dan Marino; Mary Tyler Moore; and Dr. Michael DeBakey.
Also contributing from NIH were recently retired CC nurse Louise Canada and 5NW nurse Charlotte Bosmans who judged the Issues & Ethics and Children’s Health categories, respectively.
Back to Top
Visitors from China tour CC, rehab medicine
Visitors from China were at the CC in December to exchange ideas and discuss potential collaborations in research and education. The group included representatives from the West China Medical School of Sichuan University, China’s Ministry of Health Department of Planning and Finance, and the China Southwest Architectural Design and Research Institute.
They met with Dr. Leighton Chan, chief of the Rehabilitation Medicine Department, and Dr. Li Li (far right), staff physician. Since last year’s earthquakes, China has made the development of rehabilitation medicine a priority. The government is planning a rehabilitation center—including a hospital and a clinical research laboratory—and education programs focused on resident training and in physical and occupational therapy.
The CC’s Deputy Director for Clinical Care Dr. David Henderson (fifth from left) and special assistant Laura Lee (middle) took the delegates on a tour of the Hatfield Building during their visit, coordinated by the International Society of Physical and Rehabilitation Medicine exchange committee.
Back to Top
Exhibit showcases Lasker Award winners
Members of the NIH intramural research community who have received a prestigious Albert Lasker Medical Research Award are recognized in a new exhibit on the first floor of the Clinical Center.
Mosunmola Onadipe (left) of Phlebotomy takes in the display in the hallway east of the clinic elevators. Since 1945, Lasker awards have recognized the contributions of scientists, physicians, and public servants who have made major advances in the understanding, diagnosis, treatment, cure, and prevention of human disease. Seventy-five Lasker Award recipients have gone on to win a Nobel Prize. The Lasker awards are administered by the Albert and Mary Lasker Foundation.
Back to Top
Exceptional staff honored with Director's Awards
Individual staff and project teams were recognized for exemplary service to the Clinical Center and extraordinary commitment to its mission at the NIH CC 2008 Director’s Annual Address and Awards Ceremony December 19 in Masur Auditorium. Dr. John I. Gallin, CC director, presented the awards.
Administration
Ronald J. Adams, Office of Administrative Management; Alicia R. Caffi, Office of Financial Resource Management; Janice Davis, Nursing and Patient Care Services; Rebecca Dove, Nursing and Patient Care Services; Denise Ford, Office of Organizational Development; Rozario (Tony) Francis, Office of Research Facilities Development and Operations; Julie A. Hopkins, Department of Transfusion Medicine; Madeline A. Michael, Nutrition Department; Melanie A. Reagan, Office of Administrative Management; Daniel Rinehuls, Office of Financial Resource Management; Diane Walsh, Nursing and Patient Care Services
Extramural Advisors to the Bedside-to-Bench Program: Marsha D. Mathis, Suzanne A. White, NHBLI
Commissioned Officers Dental Clinic Decommissioning Project: Michael Rice, Paula Wrenn, Materials Management Department
Jesse Ferguson Customer Service Award
Avril Bertrand, Nursing and Patient Care Services; Joe Cowling, Housekeeping and Fabric Care Department; Gary DiPatrizio, DCRI; Ann M. Ellis, Office of Administrative Management; Golnar Miamee, DCRI; Jane Thurber, Office of Financial Resource Management; Kenneth J. Williams, Office of Clinical Research Training and Medical Education
Patient Care
Ann Hickey, Nursing and Patient Care Services; David Lang, Pediatric Consult Service; Carrie Patricola, Nursing and Patient Care Services; Paul S. Plascjak, Positron Emission Tomography Department; Gladys Tataw-Ayuketah, Nursing and Patient Care Services
1 SW Behavioral Health Team: Andre Caple, James C. Gagnon, Melissa K. Maddox, Christian O. Mbulu, J. Francisco Rodriguez, Nursing and Patient Care Services
ICU Staff Team: Lincoln Farnum, DCRI; Therese R. Kent, Critical Care Medicine Department; Patricia Sengstack, DCRI; Nancy L. Munro, Critical Care Medicine Department; Daniel A. Sweeney, Critical Care Medicine Department
NIH Children’s School: Anna L. Davidson, Anita L. Fields, Susan B. Job, Helen E. Mays, Anne G. Wasson, Children’s School
Point-of-Care Testing Design and Build Team: Tony Barnes, DCRI; Yulia Broydo, DCRI; Seth Carlson, DCRI; Joshua Cohen, DLM, Tim Fink, DCRI; Barrett Grieb, DCRI; Murali Kumar, DCRI; Yenshei Liu, DCRI; Bonnie Meilinger, DLM; Betty Patterson, DLM; Nadja Rehak, DLM; Chung-Hee Row, DLM; Martha Shepherd, DASS
Robotic Surgery Nursing Team: Pawel Gawlik, Jardin (Jay) Punzalan, Ada Rivera, Juanita Washington, DASS
Science
Xizhong Cui, Critical Care Medicine Department; Migdalia V. Rivera-Goba, Nursing and Patient Care Services; Frank Witebsky, DLM
n Clinical Chemistry Service: Debra Burton, DLM; Gyorgy Csako, DLM; Steven Drake, Critical Care Medicine Department; Glen Hortin, DLM; Mark Ruddel, DLM; Patricia Sullivan, DLM
Strategic Initiatives
Leighton Chan, Rehabilitation Medicine Department; Barbara I. Karp, NINDS; Jon W. McKeeby, DCRI
Sunrise Medication Manager Design and Build Team: Andrea Beri, DCRI; Michael Brown, Pharmacy Department; Tom Dawson, DCRI; Robert DeChristoforo, Pharmacy Department; Gary DiPatrizio, DCRI; Barry Goldspiel, Pharmacy Department; Elizabeth McNamara, DCRI; Jharana Tina Patel, Pharmacy Department; Victoria Skahill, DCRI
Patient Ambassador Team: Courtney Duncan, Social Work Department; Jennifer Haliski, Office of the Director, NIH; Kathy Hilburn, Office of Administrative Management; Karen Kaczorowski, Nursing and Patient Care Services
Teaching/Training
Margaret Bevans, Nursing and Patient Care Services; Andrew J. Dwyer, Radiology and Imaging Sciences; Juan J.L. Lertora, Office of Clinical Research Training and Medical Education; Julia Locklin, Radiology and Imaging Sciences; Josanne Revoir, Nursing and Patient Care Services
IPPCR China Faculty: Dennis O. Dixon, NIAID; Laura Lee Johnson, NCCAM; Reidar Lie, Bioethics Department; Charles Natanson, Critical Care Medicine Department; Jerry A. Menikoff, Office of the Secretary, DHHS
Back to Top
New vaccine clinic marks World AIDS Day with red-ribbon cutting

|
|
 |
|
The Vaccine Research Center (VRC) Clinical Trials Core marked World AIDS Day 2008 with a red-ribbon cutting for the new Vaccine Evaluation Clinic on 5NE-S (above left).
At top right, Clinical Center Director Dr. Gallin (center) joined Clinical Trials Core Chief Dr. Barney Graham and Deputy Chief Dr. Julie Martin in welcoming the new team (above right).
The primary mission of the group is the evaluation of candidate vaccines for HIV, biodefense, and emerging and re-emerging infectious diseases in Phase I clinical trials. The new clinic welcomed patients this month. An open house is planned for February 23. For more information, visit vrc.nih.gov or call 1-866-833-LIFE (5433).
|
Back to Top
Jingle Jungle wins fifth annual gingerbread house competition
Winners of the Clinical Center’s fifth annual gingerbread house competition were announced by CC Director Dr. John I. Gallin on December 18. The contest pulled 34 entries from departments across the CC.
The houses were on display in the atrium, where nearly 2,000 votes for a favorite were cast by staff, patients, and visitors. Following the winners announcement, most houses remained inside the CC’s north entrance; some went to the Edmond J. Safra Family Lodge or the Children’s Inn. The Inn also benefited from a very successful food drive in conjunction with the gingerbread house contest.
Clockwise from top left are: first place winners for the Jingle Jungle treehouse with 487 votes, the Hospital Epidemiology Section (from left: Annette Booze, Angela Michelin, Sarah Turkel, Jacqueline Reid, Robin Odom, Maryann Bordner); second place winners for a White House replica with 273 votes, the Intensive Care Units (from left: Abby Johnson, Barbara Eaton, Rosane Suleiman, Pam Horwitz, Heather Rhine, Mary Stephens, Danelle Gawlick, Kathleen Fitzgerald, Avril Bertrand, Aileen Estoque); and third place winners for a birdhouse trifecta with 167 votes, the Department of Laboratory Medicine’s Chemistry Section (from left: Tracey Sutton, Marie Conrad, Emily Frawley, Tracey Bosworth, Perlita Powers).
Back to Top
CC podcasts air latest news online
The newest exit on the information superhighway? The brand new Clinical Center podcast—“NIH Clinical Center Radio.”
Hosted by Bill Schmalfeldt, creator of the successful “NIH Research Radio” podcast in 2006, “NIH Clinical Center Radio” shines the spotlight on the people who perform and support the research that goes on each day at America’s clinical research hospital.
Recent podcast episodes have featured the Medicine for the Public series of lectures, clinical trials being conducted at the CC, discussions on mentoring from the 2008 CIST Forum, and the kickoff of the CC’s Combined Federal Campaign efforts.
What is a podcast? Think of it as radio where you control the programming. You listen when you want to, and there are a couple different ways to do it.
Subscribe on iTunes (or whatever you use to download content on your portable MP3 player), and automatically receive the most recent episode when it’s released.
The podcast home page has more information on how to listen or subscribe to this free service of the CC’s Office of Communications, Patient Recruitment, and Public Liaison.
“Podcasting is the wave of the future,” Schmalfeldt said. “More and more government agencies are using podcasting to get out their messages. For the listener, it’s easy and convenient. For the agency, it’s inexpensive and very cost-effective. It’s a great way to let the people at the Clinical Center tell their stories in their own voices, so you can hear the passion they have for the incredible jobs they do every day.”
Back to Top
Off-campus shuttles schedules change
The NIH conducted a comprehensive review of the shuttle system examining ridership throughout the day, escalating fuel costs, and resources required to maintain a route. As a result of this review, effective January 5, the NIH made significant changes to the Executive Plaza and Mid-Pike Plaza shuttle routes and schedules.
The NIH Executive Plaza route has been decreased from three shuttles to two shuttles. Additionally, the Executive Plaza shuttle will service the Mid-Pike Plaza commuter parking lot weekdays between the hours of 10 am - 4 pm. The Mid-Pike Plaza commuter parking lot will be the first stop on the Executive Plaza route after leaving the campus. The Executive Plaza route will revert back to its regular schedule between the hours of 4 pm - 6:30 pm.
The Mid-Pike Plaza route has been combined with the Executive Plaza shuttle during the hours of 10 am - 4 pm weekdays. The Mid-Pike Plaza morning route will not change between the hours of 5:40 am - 10 am. Between the hours of 4 pm - 7 pm the Mid-Pike Plaza shuttle will revert back to only stopping at the Mid-Pike Plaza commuter parking lot. Additionally, the Mid-Pike Plaza shuttle will discontinue service to the Mid-Pike Plaza commuter parking lot at 7 pm.
There are no changes to any of the NIH Patient Shuttle Routes or to the Campus, Campus Limited, Rockledge, and Perimeter Shuttle Routes.
To view the new Executive Plaza and Mid-Pike Plaza routes and schedules and other existing NIH shuttle routes, please visit: http://dtts.ors.od.nih.gov/NIHShuttle/scripts/shuttle_map_live.asp
Back to Top
CFC basket drawing raises over $7,000
Winners of the Clinical Center’s basket drawing to benefit the Combined Federal Campaign (CFC) were chosen by 3-year-old Sydnie Gapper, a patient’s daughter from Oregon, on December 4. Raffle tickets for the 19 baskets brought in $7,047 for the CFC, pushing the CC over its goal for the year.
“This is the first time the Clinical Center has ever reached our goal before Christmas, and that says a lot in this economy,” Maureen Gormley, CC chief operating officer, told the crowd gathered in the Hatfield Building’s atrium.
Sydnie chose the tickets of winners, who included NIH staff, patients and a patient family member. The big winner of the day, Kim Scott of Nursing, won two baskets —she’ll enjoy both a dog lovers and a chocolate, tea, and coffee collection. The most sought-after basket, donated by Medical Records, contained a Wii and raised over $2,000; Leon Segears of the NIH Center for Information Technology was the lucky winner. Above, Gormley (left), Gapper, and CFC deputy coordinator Deborah Byram (right) celebrate with Dr. Adrienne Farrar, chief of the Social Work Department, after her Book Lover’s Basket win.
Back to Top
Long-time CC nurse Canada retires
Louise Canada, senior clinical research nurse in the OP10 Eye Clinic, retired on December 3.
Canada graduated from the Alexandria Hospital School of Nursing in Virginia in 1973 and earned her master of science in nursing from Catholic University. She worked as an ophthalmic nurse for 19 of her 26 years at the Clinical Center, achieving the title of certified registered nurse in ophthalmology in 1989 and recertifying in 1999 and 2007. She is one of only four CC nurses to have held this distinction.
After stints in other patient units and clinics, she returned to the eye clinic in 2000 as a clinical research nurse and coordinator. Her career also included nursing positions on a variety of medical-surgical units at the National Naval Medical Center and Naval Hospital Camp Lejuene in North Carolina.
Canada’s writing has appeared in the Endocrine Nurses Society Newsletter and in CC News, and she was a contributor to the endocrine chapter in Mosby’s Clinical Nursing, 5th Edition, published in 2001.
Other involvements include her role as the first Nursing and Patient Care Services historian, working on several history of nursing projects and posters, and participation in the American Association for the History of Nursing. For the last eight years, Canada has judged for the International Health & Medical Media Competition, known as the FREDDIE Awards. (See related story, page 4.)
After many years and many fond memories, she is looking forward to spending time with her mini-rabbit farm and friends in the Shenandoah Valley. Canada thanks the CC and NEI staff for their kind support and ongoing commitment to the preservation of sight.
“Caring for others is food for the soul,” she said.
Back to Top
NIH-Duke program taking applications
Applications are being accepted for the 2009-2010 NIH-Duke Training Program in Clinical Research. Implemented in 1998, the program is designed primarily for physicians and dentists who desire formal training in the quantitative and methodological principles of clinical research. Courses are offered at the CC via videoconference technology. Academic credit earned by participating in this program may be applied toward satisfying the degree requirement for a Master of Health Sciences in Clinical Research from Duke University School of Medicine.
The degree requires 24 credits of graded course work, plus a research project for which 12 units of credit are given. The program is designed for part-time study, allowing the student to integrate the program’s academic training with his or her clinical training. Applications are available in CC-Room B1L403. Enrollment in this program is limited; interested individuals should inquire with their NIH Institute/Center regarding funding for participation. The deadline for applying is March 1, 2009, and successful applicants will be notified by July 1, 2009. Additional information is available at http://tpcr.mc.duke.edu or by e-mail to tpcr@mc.duke.edu.
Back to Top
Participants sought for clinical research trials
More information on the following studies can be found at http://clinicalstudies.info.nih.gov or by calling 1-866-444-2214 (TTY: 1-866-411-1010).
Twins study
A clinical research study (89-M-0006) sponsored by the National Institute of Mental Health is seeking same sex fraternal twins 5-20 years of age to observe brain development in healthy children. There is no cost for study-related tests. Compensation is provided.
Overeating teens
A clinical research study (08-CH-0139) by the National Institute of Child Health and Human Development seeks girls age 12-17 at risk for becoming overweight adults through above-average weight or episodes of loss of controlled eating for a prevention study. Compensation is provided.
Pelvic pain
A clinical research study (04-CH-0056) sponsored by the National Institute of Child Health and Human Development seeks healthy women age 30-50 to investigate the role of hormones and genes in pelvic pain and explore better approaches to treatment. All study-related tests are provided at no cost. Compensation is provided.
Back to Top
Lectures & Events
Clinical Center Grand Rounds, 12pm, Lipsett Amphitheater
All lectures will be videocast at http://videocast.nih.gov.
February 4, 2009
Ethics Rounds
Are Risks to Family Members Grounds for Exclusion?
David Magnus, PhD
Director, Stanford Center for Biomedical Ethics
Associate Professor, Division of Medical Genetics, Department of Pediatrics
University of Stanford
February 11, 2009
Contemporary Clinical Medicine: Great Teachers
The Art of Failure in Medicine
Atul Gawande, MD, MPH
Surgeon, Brigham and Women’s Hospital
Associate Professor, Department of Surgery, Harvard Medical School, and Department of Health Policy and Management, Harvard School of Public Health
February 18, 2009
The Winner’s Curse: The Market for Exchange of Science
Neal Young, MD
Chief, Hematology Branch, NHLBI
Ethical Challenges for Medical Journals
Christine Laine, MD, MPH
Senior Deputy Editor, Annals of Internal Medicine
February 25, 2009
John Doppman Memorial Lecture
Oncologic Imaging: Endless Horizons
Hedvig Hricak, MD, PhD
Chair, Department of Radiology
Carroll and Milton Petrie Chair
Memorial Sloan-Kettering Cancer Center
Professor of Radiology
Cornell University
Back to Top
This page last updated on 12/14/2017


 The information on this page is archived and provided for reference purposes only.
The information on this page is archived and provided for reference purposes only.