Clinical Center News
Promising pilot study by CC researchers treats deep vein thrombosis by lacing clots
 |
Researchers who collaborated on the project stand in front of scans showing (from left) a pilot study participant’s veins before and after the alteplase treatment. (Back row, from left): Drs. McDonald Horne, DLM; Richard Cannon, NHLBI; Richard Chang, DRD; and Anthony Kam, DRD. (Front row, from left): Clara Chen, NMD; and Edie Mao, DRD. Not pictured: Thomas Shawker, DRD.
|
Clinical Center researchers have developed and published a novel treatment for blood clots in the legs that appears to be safe and effective, according to their pilot study.
Deep vein thrombosis (DVT) is a common but serious health problem that happens when a blood clot, or thrombus, forms in the deep veins, particularly in the lower leg or thigh. Complications occur when the clot breaks off and travels to the lungs, resulting in pulmonary embolism, a potentially fatal condition. Lack of movement is a risk factor for DVT, which is why long-distance airline passengers and patients who recently had surgery or were hospitalized often hear about the condition.
Most patients with DVT are treated with medications to thin the blood and compression stockings. However, studies have shown that one-third of these patients will suffer from post-thrombotic syndrome, characterized by pain, swelling, or changes in skin color. Another third are likely to have another clot or pulmonary embolism within five years of their initial DVT.
Clot-dissolving therapies could potentially protect against these occurrences, but can pose a bleeding risk. Therefore, lead author Dr. Richard Chang, chief of the interventional radiology section in the CC Department of Radiology, and colleagues in the CC Department of Laboratory Medicine and Nuclear Medicine Department sought to develop a safe, effective, and affordable clot-dissolving treatment regimen for DVT.
 |
 |
|
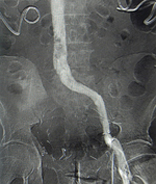
The scan on the left shows the clotting within a patient’s vein before the treatment. The scan on the right is noticeably clearer of clots.
|
For the pilot study, the researchers injected or “laced” the clots of 20 acute DVT patients with alteplase, a clot dissolving agent. Alteplase binds to the clot, so the procedure does not require continuous infusion of the drug, as do other clot-dissolving therapies. With this treatment, after lacing one vein segment with alteplase, the interventional radiologist can immediately direct catheters to treat other vein segments to ensure that the entire clot has been adequately treated. The patients also received blood thinners.
The new treatment restored blood flow throughout the deep venous system in 16 (80 percent) of the 20 patients during therapy with complete resolution of symptoms in 18 patients (90 percent) after six months of treatment with blood thinners. Alteplase left the patients’ circulatory system within two hours of treatment, reducing the risk of subsequent bleeding. “This treatment regimen is able to clear blood clots rapidly and safely, restoring blood flow in the veins of the lower leg, and the results are durable,” said Chang.
There were no cases of clinically important pulmonary embolism or serious bleeding during the treatment, and no cases of post-thrombotic syndrome or recurrent clotting during the more than three years that the researchers followed the patients. “With this therapy, pain and swelling resolve rapidly, and, in most cases, the patient is able to resume all normal activity within a week,” said the study’s co-author, Dr. McDonald Horne from the hematology section of DLM.
The CC researchers’ paper, “Deep Vein Thrombosis of the Lower Extremity: Direct Intraclot Injection of Alteplase Once Daily with Systemic Anticoagulation— Results of a Pilot Study,” appears in the February issue of Radiology, a monthly scientific journal devoted to clinical radiology and allied sciences. The authors caution that larger clinical trials are required to further support the efficacy of the treatment.
Back to Top
Curriculum broadens clinical research skills
 |
Jacquin Jones, a clinical research nurse with NCI, talks with patient Joyce Hanula about her participation in a protocol during Hanula’s monthly visit to the Clinical Center. How to communicate effectively with patients about topics related to clinical research, such as patient privacy and lab results, was one of the things Jones practiced through the clinical research curriculum that she often applies in her daily work.
|
Considering working toward the Clinical Center’s clinical research curriculum certificate, which is administered by the Office of Clinical Research Training and Medical Education? You’re in good company. Since the first certificate was awarded in November 2004, more than 50 individuals engaged in clinical research at all career levels have earned one. They include senior physicians, staff clinicians, investigators, dentists, nurses, allied health professionals, and clinical fellows.
The curriculum’s required core components include several courses: “Introduction to the Principles and Practice of Clinical Research;” “Ethical and Regulatory Aspects of Human Subjects Research;” “Clinical Research Training;” and a training course for NIH Institutional Review Board (IRB) members.
In addition, participants must complete a clinical research experience, such as attending two meetings as an ad hoc IRB member or contributing to the drafting of a protocol. One or more supplemental electives may also be completed to receive a certificate “with commendation.”
Dr. Scott Paul, a physiatrist with the Rehabilitation Medicine Department (RMD), came to the CC in 2001 from a clinical private practice setting. He wanted to increase his research skills for a clinical research environment, refresh his knowledge of statistics, and survey the clinical research process. In his current role as research coordinator for the medical staff section of RMD, Paul mentors students and advises RMD and IC investigators on designing studies that assess function and disability. He says the courses he took made both responsibilities easier and he tells fellows and students to take the introductory course.
“All the elements of this program are important,” Paul said. “If you’re coming to the CC from a clinical or laboratory setting and haven’t done clinical research before, it’s important to have a general survey of what the issues and processes are. If you haven’t been using statistics on a regular basis, it’s important to have greater statistical ‘fluency’ because you can’t get away without it. Human-subjects research involves human beings so it’s important to think through the related ethical issues. By giving you the necessary tools to be an effective and ethical clinical researcher, it makes you a better researcher. It’s an effort, there’s no question. You put in extra time, but I think you get out what you put in.”
NIA’s Dr. Basil Eldadah agrees with Paul about the value of the curriculum. He said that in his role as program officer for the Geriatrics Branch of the Institute’s Geriatrics and Clinical Gerontology Program he deals with issues directly related to the clinical research curriculum’s courses on nearly a daily basis.
Terri Wakefield, director of clinical research services for core intramural NIDDK, found that although many of the components of the program involved skills she was cultivating independently, participating in the certificate program formalized her understanding of those activities. “If you want to broaden and quantify your skills, these courses will help do this for you,” she said. Wakefield participates in the NIDDK/NIAMS IRB, which reviews protocols involving a lot of different ICs. She said the courses helped her to be more thoughtful about the protocols she considers. “Many of the training programs offered at NIH are outstanding— things most people don’t have available at their backdoor.”
The courses also provide a common language for intramural and extramural clinical researchers. NINDS’ Dr. John Lynch said the experience he gained allowed him as a primary investigator to provide critical feedback to extramural investigators. “The courses provide some baseline training that is essential to conduct clinical research,” Lynch said.
The information presented in the courses also benefits those who may pursue their career goals related to clinical research outside NIH. Dr. Nicholas DiProspero, associate director for experimental medicine at Johnson & Johnson Pharmaceutical Research and Development, was interested in developing therapeutics for neurodegenerative disorders while he was a fellow in the Clinical Pharmacology Research Associate Training (ClinPRAT) program from 2003 to 2006. DiProspero said he gained an understanding of how to approach clinical research from the courses, built upon its foundation through further study and coursework, and now uses the courses’ principles daily in the design and conduct of phase 1 and 2 trials. “There are very few places that offer a curriculum to learn the fundamentals of clinical research,” DiProspero said. “I would recommend this unique NIH program to any researcher not only to provide the insight and skills necessary to be able to conduct clinical research but also the foundation to critically interpret and extrapolate research findings.”
Jacquin Jones, a clinical research nurse with NCI, said she enrolled because she felt that as an NIH nurse it was important to increase her clinical research understanding. “I continually apply what I learned, and I feel that I have a better understanding of what protocols and principle investigators are looking for. I still have a lot to learn, but the foundation is priceless,” Jones said.
According to Jones, the certificate program will “broaden your understanding of what we are doing at NIH no matter what your level of involvement is in research. For a program that is free and given by those who are on the cutting edge of research, it was an honor to participate. Everyone will take something different away from it, but the tools that are provided will be useful references for future research.” More information is available online at http://intranet.cc.nih.gov/clinicalresearchtraining/curriculumcert/index.html.
Back to Top
‘I experienced some of what our patients’ families experience’
 |
Patience Mbulu demonstrates how she performs patient intakes with her CC nursing colleague Regina Smith-Turner.
|
Patience Mbulu, clinic coordinator for the urology branch and OP3 clinic nurse, came to the United States from Nigeria 21 years ago with only a small suitcase. She is amazed by the good things her new country, and her job at the Clinical Center, have brought to her.
“It’s a blessing to work here,” Mbulu says. “We give great nursing care and are empowered with the resources to provide the best care possible.” CC staff have recognized how Mbulu has taken advantage of those resources to provide excellent care. Her peers nominated her to be honored as nurse of the year during the CC’s 2005 Nurses Week awards ceremony.
Because of Mbulu’s work as a CC nurse, Mary Okobiemen, her niece back in Nigeria, can now live without pain for the first time in her life. Diagnosed at age two with sickle cell disease, Okobiemen was in and out of hospitals with severe pain and complications of the disease for most of her life. In her late twenties, the frequency and severity of her chest pains increased. Mbulu didn’t know what was wrong, but she knew Okobiemen needed to be evaluated again by a physician. NHLBI’s Dr. Zakari Aliyu was in Nigeria screening patients for sickle cell disease and diagnosed Okobiemen with pulmonary hypertension, a common symptom of the disease. Aliyu, together with NIDDK’s Dr. John Tisdale and NHLBI’s Dr. Mathew Hsieh, helped bring Okobiemen to the United States and the CC for a bone marrow transplant in November 2006. After treatment, Okobiemen returned to work in Nigeria.
Mbulu says experiencing her neice’s treatment at the CC from the perspective of a family member made her a better nurse to other patients. “When they had to call a code blue on her, it struck me that this was my family, my loved one. I was experiencing some of what our patient families experience. I could now tell them I know what they’re going through because I’ve been through it too. I am very grateful for the work of all the physicians and nurses who participated in her care while she was at NIH.”
Some of Mbulu’s friends don’t realize that she cares for patients as part of her job—they think she just does research. Mbulu attempts to correct these misconceptions by talking about her work and encouraging other nurses and nursing students to consider careers at NIH and the CC. Mbulu was featured in the winter issue of Montgomery College’s Insights magazine celebrating the 40th anniversary of their nursing program.
Mbulu is also a role model for continuing nursing education, and she will complete her master’s degree this May with a dual certificate in nursing education and health services leadership and management.
Back to Top
Jeter Foundation students visit NIH and CC, tour metabolic unit
 |
(back row, from left): NIDDK’s Frank Holloman; Dr. Kong Chen, director of the core laboratory on the Metabolic Clinical Research Unit; and NIDDK Director Dr. Griffin Rodgers with the visiting Jeter's Leaders students in the unit’s exercise testing room.
|
A group of teenagers from the Turn 2 Foundation, established by New York Yankees Captain Derek Jeter, on Feb. 19 visited NIH facilities and the Clinical Center, including the Metabolic Clinical Research Unit.
The foundation was created in 1996 to help inner-city high school students avoid crime, gangs, drugs, and alcohol. The name “Turn 2” is symbolic of the dramatic double play made by infielders during a baseball game. It also represents Jeter’s wish to promote healthy lifestyles among young people and enable them to “turn to” his foundation for guidance.
The Jeter’s Leaders Program recognizes students for their academic achievements, extracurricular activities, and community service. Leaders are responsible for delivering a positive message to their peers focusing on staying in school and leading alcohol- and drug-free lifestyles.
Dr. Kong Chen, director of the core laboratory on the unit, discussed nutrition and healthy lifestyles and demonstrated exercise and body composition tests for obesity. Dr. Griffin Rodgers, NIDDK director, encouraged the visitors to pursue higher education and consider scientific careers. Metabolic unit staff demonstrated exercise-testing equipment and discussed healthy lifestyle choices, such as selecting drinks with lower sugar content.
 |
(from left): Clinical research dietitians Nancy Sebring and Blakeley Dekinger show the students visiting from the Jeter Foundation the sugar content of a variety of popular drink choices.
|
This was the third time NIH hosted students from the foundation. On the same day as the CC visit, an equal number of students toured NIAAA’s facilities in Poolesville, Md. The students pictured here toured the NIAAA facilities last year and also saw NLM’s forensic science exhibit and talked with NIAAA Clinical Director Dr. Markus Heilig about alcohol treatment and research.
 |
The students also met with NIAAA Clinical Director Dr. Markus Heilig to discuss alcohol treatment research in the clinical lab on the 1SE inpatient clinic at the CC.
|
Back to Top
Emergency drill provides a learning exercise, chance to practice
 |
(standing, from left): Lori Purdie, Julie Kohn, Cheryl Fisher, Marsha Moore, Tannia Cartledge (seated, from left): Deb Parchen, Val Fiorillo, and Barb Quinn work in the nursing command center.
|
Inclement weather in the region prevents Clinical Center staff, patients, and family members from arriving or leaving Building 10. The roof of the Edmond J. Safra Family Lodge collapses and guests need to be moved to the CC. This was the scenario that CC staff members practiced on Feb. 5 during an emergency drill to test the activation of the code yellow emergency management plan.
Imagine senior leaders’ pagers buzzing, cell phones ringing, and emails streaming in to hand-held devices to tell everyone there was any emergency. Thanks to a new mass notification system, the CC practiced that scenario as well to ensure that critical communications channels provide open and immediate contact for staff during an event.
The drill is one of the ways the CC is practicing its preparations for emergency events in accordance with the Joint Commission’s six critical functions for emergency management: communications, resources and assets, safety and security, staff responsibilities, utility management, and clinical and support operations.
 |
April Thompson-Owens (center) talks with Paula Muehlbauer, Connie Kotefka, and Ann Peterson during the drill. In the background, Charles Woodlee, Michele Evans, and Bradley Rupert discuss logistics.
|
The CC “stood up” its central command center to coordinate hospital-wide logistics and communications. Staff also manned a nursing command center to coordinate patient capacity and available beds, distribute staffing assignments for the accessible labor pool, and monitor public safety. The nursing command center stayed in contact with the NIH emergency command center and responded to needs as the scenario evolved. Some staff members took on the roles of displaced or injured guests who needed medical attention or shelter.
Laura Lee, special assistant to the deputy director for clinical care, said a key objective of the drill that was extremely successful was practicing communication within departments through emails and phone trees.
All CC departments played a critical role in testing their internal communication processes, assessing staffing needs, assessing supply levels, and food and shelter needs. In addition, “the nursing staff again did a great job of determining bed availability and staffing areas in a timely manner,” she said.
A few areas to continue to practice in the future include clarifying the amount and sources of food, water, and linen supplies on hand and refining resources available in respite areas for staff, visitors, and patient families, according to Lee.
Back to Top
Nutrition Department efforts seek ecological, economic savings
 |
(from left) Food service workers Alekos Polyzos and Crystal Cavin break down breakfast trays for the dish room pulper. The team dumps food and paper items into the water flowing over the conveyor belt, which moves it forward, and stacks the dishes into a machine that washes, rinses, dries them. The pulper gurgles and thumps as it extracts the liquid from the items and chops them into tiny pieces.
|
David Folio, chief of the Nutrition Department at the Clinical Center, didn’t wake up one morning and decide to “go green.”
Rather, his eco-friendly perspective evolved over time as he read and learned through the popular press, industry literature and memberships, food service workshops and electronic mailing lists, and equipment shows and conferences about the importance of conserving both natural resources and dollars as part of a global effort to protect and preserve the environment.
Hospital food service managers across the country are questioning their practices and identifying what changes they can make to create a healthier environment in their health care communities for themselves, for their patients, and for future generations.
At the end of last year, the CC Nutrition Department began collaborating with Maryland Hospitals for a Healthy Environment (MD H2E), part of the University of Maryland’s School of Nursing. MD H2E is working with the national campaign for healthy food in health care through Health Care Without Harm, an international coalition of organizations whose mission is to transform the health-care sector so that it is ecologically sustainable without compromising patient safety or care. For more information, see http://healthyfoodinhealthcare.org.
Louise Mitchell, sustainable foods coordinator for MD H2E, said the organization’s biggest message to hospitals is to take it one step at a time. “It can be overwhelming to think of making an entire hospital environmentally friendly. We present options and discuss the issues involved in how organizations can take a next step. Pick a change that’s easy, cost-effective, improves patient or employee safety, or that you’re particularly passionate about. The desire to make and support environmentally sustainable purchases is now mainstream. People are buying these products on their own and they’re glad when they, as patients, see these things at their hospital, she said.” Eight hospitals and two health systems in Maryland have formed green teams, or multidisciplinary committees, according to Mitchell.
Folio said he questions every practice within the department and asks if it could be better in terms of saving money and helping the environment. “The Nutrition Department’s budget remains flat but food costs keep going up. The way we have been able to come in under budget for the past four years is to find ways to reduce costs. Sometimes making environmentally friendly changes can also save money,” he said. However, before adopting each proposal, Folio evaluates it to make sure it is a sound business decision, in addition to being green.
Many of the individual items the department changed were ideas presented at national industry conferences. In addition, Folio is gradually reducing the department’s carbon footprint by purchasing smaller, more energy-efficient pieces of food service equipment as older machines need to be replaced and technology improves.
 |
Food service worker Lionel Coriolan cooks a pizza in one minute with the Nutrition Department's new high-speed oven.
|
For example, with the CC’s patient room service menu, almost all foods are cooked to order. If a patient orders a side of broccoli, the vegetable is freshly steamed, not held from a larger batch cooked earlier. Specialized devices, such as the department’s new high-speed oven, combines convection, microwave, and infrared cooking technology to cook individual servings 10 times faster while using less energy and preserving nutrients and taste. With the department’s goal of delivering a patient tray within 45 minutes of a phone order, an oven that can cook a personal pizza perfectly in one minute compared to 10 minutes in a standard oven is a valuable commodity. It saves staff time and energy, as well as pleases the patient with quicker service and a better product.
The new oven is not the only eco-friendly food service equipment change. Plastic air strip curtains hang over all walk-in refrigerator and freezer doors to lower the amount of energy used and the CC electric bill. Used fryer oil is collected and recycled into biofuel. A cardboard compactor minimizes waste volume. The dish room pulper reduces 10 trash cans of food waste into one.
 |
The Nutrition Department's re-useable cup.
|
Still on the department’s wish list is the ability to use local growers to reduce the food miles that items on the patient menu travel to get from farm to plate. Two large challenges for the CC’s Nutrition Department—as well as other hospitals seeking to purchase locally grown food—in meeting this goal are continuing to ensure the safety, consistency, and reliability of food supplies. The CC’s patient menu is also not able to accommodate seasonal produce because of the multiple specialized diets’ nutritional requirements that clinical research patients require: A tossed salad needs to be the same in January or July, regardless of what’s in season.
By bridging the gap between hospital food service operators and local farmers and vendors, organizations like MD H2E are working to resolve these issues and someday make this idea a reality. Folio’s group is forming a green team to focus their upcoming efforts, such as composting food waste and biodegradable/compostable disposable paper products. Sustainable food programs, waste reduction, recycling, and energy-conservation efforts require time, planning, and sometimes an initial investment. Not every hospital is able to implement every green idea, but Folio is committed to taking small steps one at a time to find what’s right for the CC.
“It takes time to research products, analyze the business decision, and pressure distributors to offer eco-friendly products. It’s a continuous process of learning, questioning, and considering new ideas—wondering all the while what’s best for the CC mission, our patients, and the planet,” he said.
|
Item
|
Annual cost savings, if known
|
Environmental impact
|
Patient impact
|
|
1. New milk vendor
|
$6,500
|
packaged in paper, not plastic, containers
|
Recombinant Bovine Growth Hormone-free
|
|
2. Room service program
|
cost-neutral because of a decrease in food cost, which offset the increase in labor
|
reduces food waste as patients order only what they want
|
meets patient requests on demand
|
|
3. Soup broth purchased as a base, rather than cans
|
$3,800
|
4,370 fewer cans used per year
|
no difference for patients
|
|
4. Re-useable cup
|
$15,000
|
125,000 fewer disposable cups used
|
designer swirl cup is a nicer product for patients
|
|
5. Rechargeable batteries for staff pagers
|
$400 within three years after the cost of batteries and charger
|
144 fewer batteries used per year
|
no difference for patients
|
Back to Top
Retired NIH nurses reaches important blood donation milestone
 |
(from left): Department of Transfusion Medicine staff Margaret Dodson, donor resources specialist; Dr. Susan Leitman, director of blood services; and Jackie Brown, donor resources specialist, present Rosa Lee Powell with a plaque and flowers celebrating her 100th donation on Valentine’s Day.
|
Rosa Lee Powell on Valentine’s Day became the first African-American woman to make 100 whole blood donations to the NIH blood bank.
A mental health nurse at NIH for more than 15 years, Powell began donating blood when she heard that the blood bank particularly needed donations from individuals with her blood type. She then learned that as an African American, her blood donations could benefit Clinical Center sickle cell disease patients. Since then, her donations are always earmarked for a specific patient, for whom she is a match.
Sickle cell disease is an inherited blood disorder affecting more than 70,000 people in the US, most of whom have ancestors from Africa. People with sickle cell disease have red blood cells containing an abnormal type of hemoglobin, the substance that carries oxygen to the rest of the body. There is no cure for sickle cell disease, but frequent blood transfusions help manage and prevent the pain, strokes, organ damage, and other complications that accompany the condition.
According to Dr. Susan Leitman, director of blood services in the CC Department of Transfusion Medicine, the best transfusion match for an African-American patient with sickle cell disease usually comes from an African-American donor. Sometimes sickle cell patients are unable to proceed with life-saving marrow transplants because of an insufficient supply of blood from African- American donors. One in six African Americans may be a match for a specific patient. “Sickle cell patients are often young and need the blood. It extends their life,” Powell said.
According to Halanzo Wilkins, recruitment supervisor, it’s important for African Americans to know that their brothers and sisters need the support of their community, and that donating blood is one way to express that support. NIH’s treatment protocols for sickle cell disease patients are growing, so there is an ever-increasing need for African Americans in the region to support the Department of Transfusion Medicine’s sickle cell disease red cell exchange program, he said.
Powell agrees and said she hopes other African Americans will come to NIH to donate. “It’s painless and donating blood can always help somebody. It’s a good thing to do for your community. You never know who might need blood. It could be you or your family one day that needs it.”
To donate, call 301-496-1048 to make an appointment.
Back to Top
News Briefs
Two new CC department Web resources
Two CC departments—the Office of Clinical Research Training and Medical Education (OCRTME) and the Office of Organizational Development (OOD)—recently launched new Web sites. The OCRTME site, http://www.cc.nih.gov/training, includes information on training courses and programs, continuing medical education, regular events such as Grand Rounds and Great Teachers’ lectures, and other educational resources. The OOD site, http://intranet.cc.nih.gov/owmd/index.html , includes information on new monthly training classes offered by OOD staff, required NIH and CC training and competencies, and internal customer services such as reservations for conference rooms and special events. Both departments welcome questions about the programs and services described on their Web sites.
View NIH CME credits online through Johns Hopkins partnership
Through a new partnership with the Johns Hopkins University School of Medicine to jointly sponsor continuing medical education (CME) activities offered by NIH, CME credit for the NIH programs will now be awarded by Johns Hopkins. As of March 1, staff can use the CC OCRTME’s Web site, http://www.cc.nih.gov/training/cme.html, to submit a request for a record of CME credits. The Johns Hopkins Office of Continuing Medical Education, which is accredited by the Accreditation Council for Continuing Medical Education, will work with NIH CME activity directors to assure compliance with accreditation guidelines. Contact the specific CME activity director or the OCRTME at 301-496-9425 with questions.
Back to Top
New clinical research protocols
The following new clinical research protocols were approved in January:
Modulation of Pharmacologically Induced Alcohol Craving in Recently Detoxified Alcoholics, 08-AA-0058, Markus Heilig, MD, NIAAA
A Pilot Trial of WT1 Peptide-Loaded Allogeneic Dendritic Cell Vaccine and Donor Lymphocyte Infusion for WT1-Expressing Hematologic Malignancies, 08-C-0051, Alan S. Wayne, MD, NCI
Phase II Study of Metastatic Melanoma Using Lymphodepleting Conditioning Followed by Infusion of Anti-gp100:154-162 TCR-Gene Engineered Lymphocytes and ALVAC Virus Immunization, 08-C-0055, Steven A. Rosenberg, MD, NCI
Phase II Study of Metastatic Melanoma Using Lymphodepleting Conditioning Followed by Infusion of Anti-MART-1 F5 TCR-Gene Engineered Lymphocytes and ALVAC Virus Immunization, 08-C-0056, Steven A. Rosenberg, MD, NCI
Age-Related Eye Disease Study (AREDS) Follow-Up, 08-EI-0043, Emily Y. Chew, MD, NEI
Co-Infusion of Umbilical Cord Blood and Haploidentical CD34+ Cells Following Nonmyeloablative Conditioning as Treatment for Severe Aplastic Anemia and MDS Associated with Severe Neutropenia Refractory to Immunosuppressive Therapy, 08-H-0046, Richard W. Childs, MD, NHLBI
A Randomized, Placebo-Controlled, Double-Blind Pilot Study of Pioglitazone Hydrochloride in Allergic Asthma, 08-H-0047, Stewart J. Levine, MD, NHLBI
Ciliary Dysfunction as an Underlying Etiology Linking Primary Ciliary Dyskinesia with Heterotaxy and Complex Congenital Heart Disease, 08-H-0067, Cecilia W. Lo, PhD, NHLBI
Pilot (Phase I-II) Study of Valproic Acid (Depakote) for the Treatment of the Autoimmune Lymphoproliferative Syndrome (ALPS), 08-I-0053, V. Koneti Rao, MD, NIAID
A Phase III, Multicenter Placebo-Controlled, Randomized, Double-Blind Study to Evaluate Safety and Efficacy of PROCHYMAL[TM] Intravenous Infusion for Induction of Remission in Subjects Experiencing Treatment Refractory Moderate to Severe Crohn's Disease, 08-I-0063, Peter J. Mannon, MD, NIAID
A Phase I Study to Evaluate the Safety and Immunogenicity of an Ebola DNA Plasmid Vaccine, VRC-EBODNA023-00-VP, and a Marburg DNA Plasmid Vaccine, VRC-MARDNA025-00-VP, in Healthy Adult, 08-I-0065, Julie E. Martin, DO, NIAID
PET Test/Retest Brain Imaging of Cannabinoid CB1 Receptors Using [11C]MePPEP, 08-M-0048, Robert B. Innis, MD, NIMH
Imaging of Cannabinoid CB1 Receptors Using [18F]MePPEP-d2, 08-M-0049, Robert B. Innis, MD, NIMH
Brain and Whole Body Imaging of P-Glycoprotein Function using [11C]dLop, 08-M-0062, Nicholas Seneca, NIMH
HHV6B in Epilepsy Imaging and CSF Studies, 08-N-0027, William H. Theodore, MD, NINDS
A Prospective Natural History Study of Patients with Neurofibromatosis Type 2 (NF2), 08-N-0044, Russell R. Lonser, MD, NINDS
Investigation of the Dopamine System in Frontotemporal Dementia, 08-N-0045, Edward D. Huey, MD, NINDS
Back to Top
Upcoming Events
March 5, 2008
Neurologic Manifestations of von Hippel-Lindau Disease
Russell R. Lonser, M.D.
Investigator, Surgical Neurology Branch, NINDS
John A. Butman, M.D., Ph.D.
Staff Neuroradiologist, Diagnostic Radiology Department, CC
March 12, 2008
Great Teachers
The Modern World of Foodborne Disease
Michael T. Osterholm, Ph.D., M.P.H.
Professor, School of Public Health Director, Center for Infectious Diseases Research and Policy University of Minnesota
March 19, 2008
Interferon Treatment of Hepatitis C: Is Resistance Futile or in the Designer Genes?
Jake Liang, M.D.
Chief, Liver Diseases Branch, Division of Intramural Research, NIDDK
Management of Inferferon Non-Responders: Results of the HALT-C Trial User
Marc Ghany, M.D.
Staff Clinician, Liver Disease Branch, Division of Intramural Research, NIDDK
March 26, 2008
Childhood Onset Schizophrenia: Insights from Neuroimaging Studies
Nitin Gogtay, M.D.
Staff Clinician, Child Psychiatry Branch, NIMH
Attention-Deficit/Hyperactivity Disorder: Developmental Delay or Deviance?
Philip Shaw, M.D., Ph.D.
Staff Clinician, Child Psychiatry Branch, NIMH
Back to Top
Clinical Center News, National Institutes of Health, Building 10, 10 Center Drive, Room 12C440, Bethesda, MD 20892-1504. Tel: 301-496-6787. Fax: 301-402-2984. Published monthly for CC employees by the Office of Communications, Patient Recruitment, and Public Liaison. News, article ideas, calendar events, letters, and photographs are welcome.
Back to Top
|
This page last updated on 12/14/2017


 The information on this page is archived and provided for reference purposes only.
The information on this page is archived and provided for reference purposes only.