Clinical Center News
Trans-NIH Undiagnosed Diseases Program to help name patients' puzzling conditions
 |
(from left): Dr. William Gahl, clinical director of the National Human Genome Research Institute; Dr. John I. Gallin, director of the Clinical Center; Amanda Young, a special representative from the patient community; and Dr. Stephen Groft, director of the Office of Rare Diseases, at the launch of the Undiagnosed Diseases Program.
|
by Jenny Haliski
Patients with symptoms that the medical profession has been unable to understand and treat have a new place at NIH where they can turn for help and hope in finding a diagnosis.
That’s because on May 19, the NIH Office of the Director, Office of Rare Diseases (ORD), the Clinical Center (CC), and the National Human Genome Research Institute (NHGRI) launched the Undiagnosed Diseases Program. A trans-NIH initiative, it will focus on the most puzzling medical cases referred to the CC by physicians across the nation.
According to the Genetic and Rare Diseases Information Center, which is funded by NHGRI and ORD, 6.6 percent of inquiries in the past three years were related to undiagnosed diseases. A 1989 report of the National Commission on Orphan Diseases found that that although about 50 percent of patients in the U.S. received a diagnosis in less than a year, 31 percent waited between one and five years to obtain a diagnosis, and 15 percent waited more than five years for a diagnosis.
“A small number of patients suffer from symptoms that do not correspond to known conditions, making their care and treatment extraordinarily difficult. However, the history of biomedical research has taught us that careful study of baffling cases can provide new insights into the mechanisms of disease—both rare and common,” said NIH Director Dr. Elias A. Zerhouni. “The goal of NIH’s Undiagnosed Diseases Program is two-pronged: to improve disease management for individual patients and to advance medical knowledge in general.”
To kick off the program, Dr. William Gahl, clinical director at NHGRI; Dr. John I. Gallin, director of the CC; Dr. Stephen Groft, director of ORD; and Zerhouni held telebriefings with representatives of almost 100 patient advocacy groups, which often serve as a source of information and support for people struggling with mysterious ailments, and more than 25 media representatives.
They were joined by a special speaker from the patient community, Amanda Young (see sidebar with Amanda's story). She is ecstatic that the program will help others like her. “This is the most exciting news that anyone with an undiagnosed disease could hear: Someone is going to try to help you," Young said.
“We hope to build upon our strong working relationships with many patient advocacy groups. These organizations provide a crucial link in our nation’s efforts to improve human health through biomedical research,” said Groft. “We hope that this new partnership of NIH researchers, advocacy groups, and patients will give hope for many Americans who now face troubling medical symptoms with no clear diagnosis.”
To evaluate each patient enrolled in the new program, a cadre of NIH's senior attending physicians will dedicate their expertise across numerous medical specialties. Gahl, who is an expert on rare genetic diseases, will serve as director of the new program. "We have developed a stringent referral process to ensure this program deals with those cases that have truly confounded medical experts. We will be very selective when it comes to patient eligibility. Our focus is strictly on conditions that have not been diagnosed.”
To be considered for this NIH pilot program, a patient must be referred by a physician and provide all medical records and diagnostic test results requested by NIH. Patients who meet the program’s criteria—as many as 100 each year—will undergo additional evaluation during a visit to the CC that may take up to a week.
Two nurse practitioners will manage patient recruitment and logistics for the program, which will leverage existing NIH facilities and staff.
The program's launch coincided with the 25th anniversary of Orphan Drug Act, the 25th anniversary of the National Organization for Rare Diseases, the annual meeting of the International Conference on Orphan Diseases and Orphan Drugs, and a conference on "The Orphan Drug Act at 25 Years: Retrospective and Future Views," hosted by the FDA and the Drug Information Association.
For more information, go to: http://rarediseases.info.nih.gov/Undiagnosed. Physicians and patients with specific inquiries may call the CC's Patient Recruitment Call Center at 1-866-444-8806.
Call Center staff received nearly 300 calls from potential participants and referring physicians during the program's first two weeks. The first patients are expected in July.
Patient finds answers at the Clinical Center
 |
CC Director Dr. John I. Gallin and his patient Amanda Young at the program's launch.
|
by Maggie McGuire
Amanda Young, 26, of Conyers, Ga., lived her young life as a mystery. Seeking an explanation for having contracted spinal meningitis, gas gangrene, salmonella poisoning of the sinuses, an abdominal abscess, and more, Amanda finally found an answer at the Clinical Center.
Years of intensive testing led to a diagnosis of an IRAK-4 deficiency. An extremely rare genetic mutation affects her body's ability to create a protein needed to fight bacteria, leaving her vulnerable to life-threatening infections. The oldest of only about 20 patients known to have the deficiency, Mandy seems to have put the worst behind her.
Her first years were marked by three cases of meningitis and an abdominal abscess the size of a cantaloupe. Doctors couldn't tell Mandy's parents, Lisa and Speed Young, why their daughter was brought to the brink of death every few months.
Desperate for answers, the Youngs traveled across the Southeast visiting doctors and researchers. There were no answers.
At age 8, Mandy faced another devastating illness. A cut on her leg did not heal correctly and she developed a massive infection caused by toxin-producing bacteria. The toxin-gas gangrene-forced a complete amputation of her left leg and hip.
"The infection spread faster than they could get the lab test results back. It was horrible, simply horrible. Because the gases were moving up her leg so quickly, doctors amputated the entire leg through the hip joint. She was hospitalized for months," Lisa Young remembers.
Though frustrated, the Youngs were far from giving up hope. A doctor in Atlanta recommended the case to Dr. John I. Gallin, now CC director.
In August 1990, Mandy made her first of many visits to NIH. She traveled here every six weeks for blood tests and studies, then once every three months, to twice a year. "I've been sort of a lab rat for years. But that's the only way that they can help me. And it's okay with me. I love the fact that I am making a contribution to science and to myself at the same time. I would much rather it be me, than someone else," Mandy said.
"On May 13, 2003, at 8:24 a.m., Dr. Gallin told us, 'Congratulations! At long last we have figured out the basis of Amanda's problem.' I began to shake, and the tears wouldn't stop," Lisa said. After 21 years of questions, Mandy had an answer. The meeting where the team of researchers who had worked on her case revealed their finding to the Youngs was an emotional one. "We were in shock, then ecstatic," Mandy said. "Dr. Gallin promised he wouldn't give up on me, and he didn't. After 13 years of intensive studies, my immune deficiency had a name."
The CC exists for people like Mandy and her parents, Gallin said. "Our patients are partners in medical discovery. They call this the House of Hope. Our commitment to them is to marshal medical and scientific expertise, resources, and care in the search for answers. In a research setting, one patient's answers often generate new avenues for medical advancements that ultimately help others." Mandy has more to be happy about these days.
Mandy's condition seems to improve as she ages. While the gene defect has been found, research continues into the cause, treatment and cure of the IRAK-4 deficiency. Mandy must be acutely aware of her body, as the smallest ache or sense of fatigue could mean a fatal infection has grown without detection.
Entering a career in motivational speaking, Mandy is positive about her future. She looks forward to visiting her Clinical Center "family," and is ecstatic that the NIH Undiagnosed Diseases Program will be in place to help others like her.
"This new program will be more than a place for families to come for help," Mandy said. "It will be their place to come for hope."
Back to Top
Housekeeping staff named CC patient safety champions
 |
|
(from left, standing): Latiff Yacoob, Donald Bryant, George Kennedy, Dr. David Henderson, Roger Rizer, Ronald Jones, Nathan Grey, and Angela Michelin. (from left, seated): Fikirte Gebremichael, Belaynesh Bekele, Abeba Syefu, Sonia Vaquiz, and Teresa Guevara.
HFCD team members not pictured: Teresa Scheler, Larry Williams, Maria Bommarito, Florencia Zaldivar, Annette Poindexter, Teresa Fuentes, and Selina Gyimah.
|
The Housekeeping and Fabric Care Department (HFCD) received the CC’s fourth Patient Safety Champion Award, which is given annually to individuals or teams demonstrating a sustained commitment to a safe patient environment.
From May to November 2007, the Clinical Center experienced an outbreak of Acinetobacter baumannii. According to Dr. David Henderson, deputy director for clinical care, it is a very resistant organism that can survive for extended periods—even weeks—and is hardier than some other organisms.
Managing an outbreak with such an organism requires a coordinated team approach. In addition to aggressive medical and nursing care, special attention to the patient care environment is essential. In response to this challenge, the housekeeping team received additional training, applied innovative cleaning practices far more stringent than typical in a patient-care unit, and maintained a positive attitude. Their efforts sanitized every single item in affected patient rooms with one thorough cleaning. HFCD built quality assurance checks into the process before repeating cleaning tasks and followed up with a second quality assurance check.
HFCD Chief Rob Mekelburg said the intensive cleaning, combined with the communication and education efforts from the entire patient-care team, were instrumental in eliminating the organism at the CC. “We’re proud of our housekeeping team and their important role in containing this organism, as well as their ongoing, overall contribution to the patient-care team,” Mekelburg said.
When notifying HFCD of their award, Henderson thanked the team on behalf of CC patients for their efforts. “Acinetobacter baumannii often infects the sickest, weakest patients who are least able to fight off an infection—often those in the ICU. The HFCD team had to come up with ideas beyond conventional strategies to quickly solve this patient-care issue. This involved a lot of extra work and training,” Henderson said, noting that the CC has not identified a single isolate since early December 2007 and developed a strategy in case of a recurrence.
Back to Top
NIH works up a sweat at first annual Take a Hike Day
 |
Take a Hike Day participants head off to the starting line.
|
About 2,000 NIHers participated in a non-competitive walk and fun run on May 6. The NIH Office of Management—in partnership with the Office of Research Services, Division of Amenities and Transportation Services, and the NIH Clinical Center—coordinated the event, which was held in conjunction with the 2008 National President’s Challenge and the HealthierFeds initiative.
The first 1,000 employees to register online received a commemorative “Take a Hike Day” T-shirt. The yoga warm-up on the front grounds of Building 1 drew an increasing crowd throughout the morning.
Melissa Johnson, president of the President’s Council on Physical Fitness, provided the opening remarks. Runners left first, followed by walkers. The group proceeded down Wilson Drive to the NIH perimeter pedestrian pathway and circled the campus one time, a distance of almost three miles.
In the words of Keith Ball, a health physicist in the Office of the Director:
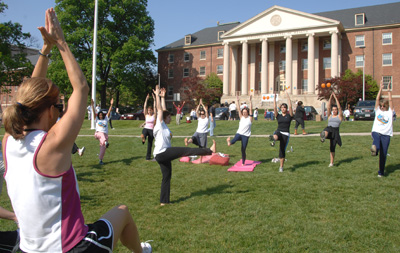 |
|
(at left, foreground): CC Chief Operating Officer Maureen Gormley strikes a pose during the morning yoga warm-up in front of Building 1.
|
Take a Hike Day
On this sixth of May
Three and a quarter miles
Was not such a long way
Plenty of volunteers there to stay
To assure that we did not swoon or sway
Water there to refresh so our day did not turn into gray
Oh, but how our muscles will surely pay
Well, we did not finish last
Nor did we finish fast
But we all sure had a blast
And no one ended up in a cast.
 |
|
(from left): Joe Hendrey (MRD) and Kathy Herring (OD) were a few of the CC staff who volunteered at the event. Water distribution stations dotted the route.
|
Back to Top
Cardozo patients come to campus for clinical needs best met here
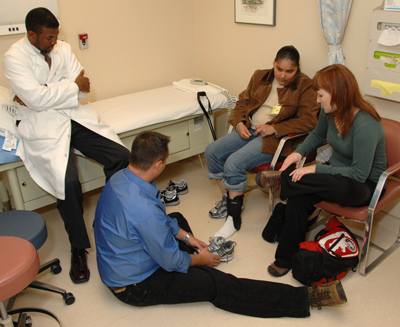 |
CC Rehabilitation Medicine physiatrists Dr. Galen Joe and Chris Gracey check the fit of the shoe inserts they created for Cardozo patient Ivania Castillo, while patient liaison Jennifer Walters translates the non-medical logistics of the visit for Castillo. Because she has both rheumatoid and osteoarthritis in her ankles, Castillo needs inserts for her shoes that are custom-molded to her foot.
|
by Jenny Haliski
Editor's note: This is the third in a three-part series on NIH's relationship with Cardozo Community Health Center. The first and second segments are in the April and May editions of the Clinical Center News.
What’s the future of the Cardozo-NIH relationship? The Health Partnership Program (HPP)’s original purpose was to conduct rigorous community-based research while asking questions that are relevant to the community. The HPP partners bring their experience and knowledge of their communities, and NIH staff contribute training and medical and research expertise for specific health conditions.
Begun in 2001, the HPP established a site in the Upper Cardozo Community Health Center of Unity Health Care, Inc. The NIAMS Community Health Center (CHC) is an extension of NIAMS’ clinical program on the NIH campus. Through the program, NIH staff have enrolled, treated, and referred patients to clinical research protocols; trained students and fellows; developed and disseminated English- and Spanish-language health education materials; and written and presented research papers, abstracts, and posters at local and national levels.
Still, there is more work to do. HPP is now implementing a five-year plan to address goals and objectives; extending the partnership to other sectors of the community while strengthening relationships; promoting new community research at the CHC; and developing new publications. Says NIAMS IRP Clinical Director Dr. Daniel Kastner, “The HPP continues to grow by extending the partnership to other sectors of the community while strengthening relationships, promoting new community research at the CHC, and developing new publications.”
NIH staff shared the lessons they’ve learned from their ongoing relationship with HPP partners through many presentations and publications in the hopes of assisting other community-based research programs. Many health professionals in and outside the Washington, DC-area benefited from this sharing of expertise on how to set up a clinic in an underserved neighborhood, how to form community partnerships, how to evaluate research programs, and how to develop effective health education materials.
Cardozo’s neighborhood is also changing. Like several other neighborhoods in the district, Columbia Heights is in the midst of a dramatic revitalization process. In some cases, new commercial development and condominium buildings are pushing long-term residents, many of them minorities, out of their rental units and away from the faith and social communities that made the area their home. According to NIH program organizers, those networks were also an important reason why the CHC was located there. As these former neighborhood residents are displaced to suburbs, they wonder if patients will return to the CHC. How will the demographics of the clinic change?
“The good thing is, the clinic is next to the Metro. The bad thing is, people tend to seek medical care close to their homes,” said Dr. Barbara Mittleman, former NIAMS director of scientific interchange and current director of the Office of Science Policy’s public-private partnership program.
 |
NIAMS patient liaison Jennifer Walters talks with Cardozo patient Maria Quevedo as she waits in phlebotomy for her blood work.
|
One way NIH has met patients where they live is through its satellite center in the Congress Heights neighborhood of Southeast DC. According to Mittleman, the patient population seeking primary care at this Unity Health Care clinic is almost entirely African American and has very limited access to health services for subspecialty care. Mittleman and a fellow visit Congress Heights every other week to see patients referred by their primary care physicians for potential rheumatic disease problems. She often refers those eligible for enrollment to the protocol underway at the CHC and offers advice to their physicians. “Some of these patients have never been to Northwest DC, let alone the NIH in Bethesda,” she said.
Another way that the NIAMS community has addressed transportation and logistical concerns is to bring CHC patients to NIH when necessary. A bus brings patients to the Clinical Center every Tuesday for access to the state-of-the-art technologies, therapies, and medications unavailable at the clinic. A fully bilingual patient liaison accompanies the visiting patients during their time at the CC and serves as a valuable resource and advocate throughout the day.
On one typical Tuesday, five CHC patients are visiting the CC. Only one speaks English, so the four Spanish speakers rely on NIAMS patient liaison Jennifer Walters to translate the logistics of their visit and a CC volunteer certified as a Spanish language interpreter for their medical interactions. A possible reflection of the evolving Cardozo area, only one of the five lives in the CHC neighborhood; the rest live in Silver Spring or Langley Park, where there are also large Hispanic communities. All have rheumatic diseases and say that the treatments they’ve received through the CHC helped their conditions to improve. Most of them heard about the clinic through friends, and would recommend that others they know participate in research because of their positive experiences. For Maria Quevedo, the opportunity to receive no-cost medical care from a place as well known as NIH factored into her decision.
“Bringing NIH to them is an important way that NIH can reach out to these populations,” said Dr. Christine Grady, head of the Section on Human Subjects Research in the CC Department of Bioethics. “In addition to providing access to diagnostic and treatment services, coming to campus helps bridge the cultural divide. People see what happens here, and they’ll go back to their community and talk to their friends and family about it.”
Back to Top
Bioethics staff publish text on clinical research with humans
 |
|
(from left): Reidar Lie, Dr. David Wendler, Dr. Christine Grady, Dr. Franklin Miller, and Dr. Ezekiel Emanuel. Not pictured: Robert Crouch.
|
Members of the Clinical Center Department of Bioethics recently edited and published "The Oxford Textbook of Clinical Research Ethics," a comprehensive textbook on the ethics of research with human beings, according to Bioethics Chair Dr. Ezekiel Emanuel. “We wanted the definitive text that assesses the history of research and the elements necessary for making research ethical such as risk-benefit ratio, informed consent, conflict of interest,” Emanuel said.
The textbook includes 73 chapters by 87 contributing authors addressing topics including a selected history of research with humans; codes, declarations, and other ethical guidance for research with humans; the context, purpose, and value of clinical research; scientific design; participant selection; risk-benefit assessments; independent review and oversight; informed consent; respect for human research participants; multinational research; and clinical investigator behavior.
According to Emanuel, Department of Bioethics faculty, fellows, and past fellows wrote nearly one third of the chapters, and fellows or former fellows co-authored five chapters.
The work is dedicated to CC Director Dr. John I. Gallin, “whose vision and continuing support made the Department of Bioethics at the NIH—and, as a consequence, this textbook—possible.”
CC staff who edited the work included Emanuel; Dr. Christine Grady, head of the section on human subjects research; Reidar K. Lie, head of the unit on multinational research; Dr. Franklin G. Miller, a bioethicist with NIMH’s Intramural Research Program and the CC; and Dr. David Wendler, head of the unit on vulnerable populations. Robert A. Crouch from the Poynter Center for the Study of Ethics and American Institutions at Indiana University also edited the work.
Back to Top
Week celebrates science, practice of clinical research nursing
 |
(from left): Linda Tondreau, who donned a Pink Panther costume for the nurse education fair, and Deb Gutierrez brought a vivid visual image to seeking out nursing performance improvement efforts.
|
Each year, the Clinical Center honors the more than 1,000 nurses who are committed to fulfilling the unique needs of the agency’s public health mission with a week-long celebration sponsored by Nursing and Patient Care Services. The CC interpretation of the American Nurses Association’s 2008 theme, “Nurses Making a Difference Everyday,” emphasized the broad impact that nurses, especially those involved in clinical research, have on how patients receive health-care treatment.
Dr. Patricia A. Grady, director of the National Institute of Nursing Research (NINR) and one of the speakers at the week’s opening ceremony, reflected on “how exciting and complicated it is to be a clinical research nurse at the CC—one of the most important places in the world because it’s where ideas are developed and tested, a place where you know you’re making a difference all across the country and the world.”
 |
Dr. Donna Berry, vice chair for research and the Myrene C. McAninch term professor in nursing at the University of Washington's School of Nursing, opened the week of celebration with her keynote address.
|
Dr. Donna Berry, vice chair for research and the Myrene C. McAninch term professor in nursing at the University of Washington’s School of Nursing, opened the celebration with her keynote address, “Patient-Centered Technologies—Making a Difference in Patient Care.”
According to Berry, an opportunity exists to begin moving patient-clinician interactions to times and places that are more convenient to patients. For example, Berry and her team developed electronic questionnaires that could be answered at home through the Web or in clinic waiting rooms with a laptop to shift when and where intake interviews occur. The idea, developed by nurses, offers a way to enhance the process of intake. The data collected provides clinicians a snapshot of each patient’s most pressing symptoms.
 |
(from left): Dr. Clare Hastings, chief of Nursing and Patient Care Services, played a board game of nursing career pathways with Dolores Medina and Brenda Justement at the nurse education fair.
|
On Wednesday and Thursday, staff visited the 1SE patio for an interactive nurse education fair with stations highlighting topics including CRN 2010, the Public Health Service, nutrition, shared governance, and ideas for broadening professional development.
Also on Wednesday, Dr. Margaret Bevans and Sandra Mitchell, both of the CC Nursing Department, presented CC Grand Rounds on issues related to hematopoietic stem cell transplants. At the opening ceremony, CC Director Dr. John I. Gallin called this lecture a “landmark” Grand Rounds because it marked the first time in the series that CC nurse scientists presented their research conducted at the CC. “The nurses make this place so special and make it work on a daily basis,” Gallin said.
The specialty practice of CRN was the theme of the presentations at the closing ceremony. Dr. Clare Hastings, chief of Nursing and Patient Care Services, said that other nurses involved in clinical research around the country and across the world were waiting for someone to clearly define the CRN role. “The CC leads the US in developing the specialty practice model for CRN, so it’s appropriate for us to define CRN roles and contributions and develop and disseminate practice documentation, standards, and management tools,” she said.
 |
|
(from left): Caroline Stewart, chair of the Recognition & Retention Committee; Tanjanell Simon, co-chair of the 2008 Nurses' Week celebration; 3NW team members Amynah Pradhan, Sten Witzel, Marie Thompson, Candice Cottle, Lisa Hancock, Joan Maher, Reema Chadid, Sue Johnson, Jaimee Pollitt, Debra Nixon-Jones, Emelli Risos, Christine McGowan, Lori McIntyre, and Barb Rawlings; and Dr. Clare Hastings.
|
According to Hastings, the long-term outcomes for the CC’s CRN 2010 initiative include:
- Defining the practice domain;
- Establishing practice standards;
- Determining core competencies;
- Developing content for the certification process; and
- Creating tools to assist CRNs in specialty practice development and documentation.
Chad Koratich, special assistant to Dr. Gwenyth Wallen, chief of the Research and Practice Development Service, and Kate Castro, clinical nurse specialist on 3NE, also spoke about CRN 2010. Castro shared from the perspective of the 2010 nursing teams who interviewed CC nursing staff across all units and clinics about the five dimensions of CRN, including study management, clinical practice, care coordination and continuity, contributing to the science, human subjects protection. Koratich said CRN 2010 is an opportunity for CC nurses to capitalize on their expertise in the five domains and grow professionally in areas outside clinical practice if they choose.
 |
(from left): Tanjanell Simon; Caroline Stewart; OP8 team members Amy Nelson, Liz Formentini, Rose McConnell, Jakki Plummer, Barbara Corey, Margie Lloyd, Jean Hammer, Sten Witzel (former), France Sundt, Brent Bonfiglio, and Gregg Roby; and Dr. Clare Hastings.
|
3NW received the “Best Collegial Practices” Patient Care Area Award, which was given this year instead of the Nursing Team Excellence Award. OP8 received the second place award. Criteria for the award, which is intended to emphasize and celebrate teams’ cohesiveness and nurturing themselves and others, included professional development; communication and collaboration; staff retention; workplace cohesiveness; team work; and appreciation.
Also nominated for the award were 1SW, 7SWN, 1SE pediatric clinic, 5SE, OP4, 3NE, and 3SWS.
CC nursing staff recognized with national awards
Dr. Margaret Bevans, clinical nurse scientist in Nursing Research and Practice Development, CC Nursing and Patient Care Services, received the 2008 RADM Faye G. Abdellah Publication Award for Nursing Research from the Nurse Professional Advisory Committee of the US Public Health Service. The award recognizes her work in addressing health-related quality of life in patients receiving reduced intensity conditioning allogeneic hematopoietic stem cell transplantation.
The committee also named Keith Marin, clinical research nurse on 3NW, and Paula Muehlbauer, clinical nurse specialist in surgical oncology, 2008 co-recipients of the RADM O. Marie Henry Publication Award for Clinical Practice. The award is in recognition of their work on intraperitoneal chemotherapy used for peritoneal carcinomatosis and ovarian cancer, techniques for assessing the peritoneal space, and the nursing management of side effects associated with this treatment.
Bevans, Marin, and Muehlbauer received their awards at Nurse Recognition Day on May 2 in Lister Hill Auditorium.
In other nursing awards news, a poster by Kaylan Fenton and Amanda Funkhouser-James, clinical research nurses on 7SW-N, on the use of a newly available IV medication for status epilepticus won third place at the American Association of Neuroscience Nurses Annual Conference in Nashville, Tenn.
DASS staffer places third in run at perioperative nurse conference
Ruth Nunes, a perioperative staff nurse in the Clinical Center’s Department of Anesthesia and Surgical Services, was one of three department staff who presented posters at the 2008 Association of periOperative Registered Nurses (AORN) Congress in April in Anaheim, Calif., along with Nancy Diaz and Carrie Minard.
The conference includes an annual AORN Foundation 5K Fun Run/Walk to raise funds for educational scholarships. Nunes ran the April 2 race and placed third in her age category, while wearing her NIH shirt.
Back to Top
Pain, Palliative Care team tea parties a spa for CC patients’ souls
 |
Around the tea table are (from left): Dr. Ann Berger, Larry Bauer (OCPRPL), Jayne Phillips, Dr. Dan Handel, Karen Baker, Dr. Eric Bush, and Dr. Jacques Bolle.
|
The CC Pain and Palliative Care team gives countless tea parties for critically and terminally ill CC patients. Mothers and daughters, married couples, and pediatric patients and their families have all donned hats and boas, sipped tea, and sampled dainty treats over the years.
On May 6, the group toured the Washington National Opera’s rehearsal and costume studios in Takoma Park as part of a team-building retreat organized by Larry Bauer in the CC Office of Communications, Patient Recruitment, and Public Liaison. After their tour, the group tried on costumes and held a tea party of their own celebrating their work and the patients they have served throughout the years.
“Tea parties can have a therapeutic value because they change the milieu for the patient. Suddenly, it’s not a hospital or ICU room for a few minutes,” CC nurse practitioner Karen Baker said. Dr. Dan Handel said his favorite part of the department’s service is the first five minutes when the patient doesn’t yet register that the tea party is for them, they’re surprised, and then realize how deeply their caregivers are there to support them.
Every tea party is memorable for Pain and Palliative Care Chief Dr. Ann Berger. “It changes our interaction with the patient from ‘tell me about your pain’ to celebrating their life. It also can bring cheer to the CC staff to see us rolling down the hall with the tea cart,” she said.
As the group read quotes about tea, one by contemporary author, philosopher, and interior designer Alexandra Stoddard stood out as representing their mission for CC patients. “The tea party is a spa for the soul. You leave your cares and work behind. Busy people forget their business. Your stress melts away, your senses awaken.”
Back to Top
Pharmacy Information System
 |
(from foreground): CC pharmacy staff Mary Byrne, Jessica Weintraub, and Justine Harris participate in the pharmacy training session.
|
The Clinical Research Informatics and Pharmacy Departments implemented the first phase of a new pharmacy information system (Sunrise Medication Manager, or SMM) in May. Developed as an integrated component of CRIS, the Clinical Research Information System, SMM will enhance the efficiency, safety, and processes of medication management at the CC. The first phase involved primarily oral medications.
Training will be an on-going priority throughout the pharmacy’s information system project.
Back to Top
New clinical research protocols
The following new clinical research protocols were approved in April:
Effect of Naltrexone on Craving and Ethanol-Induced Brain Activity, 08-AA-0125, David T. George, MD, NIAAA
A Phase 2 Trial of Tandutinib in Combination with Bevacizumab for Patients with Recurrent High-Grade Gliomas, 08-C-0101, Howard A. Fine, MD, NCI
Phase II Study in Patients with Metastatic Melanoma Using a Non-Myeloablative Lymphocyte Depleting Regimen of Chemotherapy Followed by Infusion of gp100 Reactive Peripheral Blood Lymphocytes (PBL) and High or Low Dose Aldesleukin, 08-C-0104, Udai S. Kammula, MD, NCI
Natural History Study of Monoclonal B Cell Lymphocytosis (MBL) and Chronic Lymphocytic Leukemia/ Small Lymphocytic Lymphoma (CLL/SLL), 08-C-0105, Wyndham H. Wilson, MD, NCI
Phase II Study of Metastatic Cancer that Expresses NY-ESO-1 Using Lymphodepleting Conditioning Followed by Infusion of Anti-NY ESO-1 TCR-Gene Engineered Lymphocytes, 08-C-0121, Steven A. Rosenberg, MD, NCI
A Phase 1, Single Center, Dose Escalation Study of CAT-8015 in Children, Adolescents and Young Adults with Refractory CD22+ Acute Lymphoblastic Leukemia (ALL) or Non-Hodgkin's Lymphoma (NHL), 08-C-0123, Alan S. Wayne, MD, NCI
A Phase I Combination Study of AZD2281 and Cisplatin Plus Gemcitabine in Adults With Solid Tumors, 08-C-0128, Martin E. Gutierrez, MD, NCI
Communicating a Cancer Diagnosis: Current Methods and Their Effects, 08-CC-0127, Ezekiel J. Emanuel, MD, CC
Hepatitis C Eradication and Progression of Atherosclerosis, 08-DK-0106, Yaron Rotman, MD, NIDDK
Screening Study for the Evaluation and Diagnosis of Potential Research Participants, 08-EI-0102, Frederick L. Ferris III, MD, NEI
High Speed Indocyanine Green Angiography Findings in Induction/PRN Regimen of Intravitreal Ranibizumab Injection for Neovascular Age Related Macular Degeneration, 08-EI-0103, Catherine Meyerle, MD, NEI
Effects of Worksite Wellness Interventions on Vascular Function, Insulin Sensitivity and High-Density Lipoprotein in Overweight or Obese Women, 08-H-0108, Richard O. Cannon III, MD, NHLBI
Patient Provider Communication and Interaction in a Virtual Clinical Setting, 08-HG-0122, Susan Persky, PhD, NHGRI
Back to Top
Upcoming Events
June 4, 2008
Targeted Approaches to Therapy for X-Linked Hyper IgM Syndrome
Ashish Jain, MD
Chief, Clinical Immunology Unit, Laboratory of Host Defenses, NIAID
Syndrome Management of Atypical Mycobacterial Infections
Steven M. Holland, MD
Chief, Laboratory of Clinical Infectious Diseases, NIAID
June 11, 2008
Great Teachers: John Laws Decker Memorial Lecture
Solving the Inflammation Puzzle One Patient at a Time
John I. Gallin, MD
Director, CC
Lecture will be videocast, http://videocast.nih.gov
June 18, 2008
The Evolving Impact of Pneumocystis on Human Health: A Century of Progress
Henry Masur, MD
Chief, Critical Care Medicine Department, CC
Joseph Kovacs, MD
Senior Investigator, Critical Care Medicine Department, CC
Attending Physician, HIV/AIDS Program, NIAID and CC
June 25, 2008
Qualitative Features of an Effective Immune Response to HIV-1
Mark Connors, MD
Chief, HIV-Specific Immunity Section, Laboratory of Immunoregulation, NIAID
Stephen Migueles, MD
Staff Clinician, HIV-Specific Immunity Section, Laboratory of Immunoregulation, NIAID
Back to Top
This page last updated on 12/14/2017


 The information on this page is archived and provided for reference purposes only.
The information on this page is archived and provided for reference purposes only.